◒
De Quervain Injection
From WikiMSK
This article is still missing information.
| De Quervain Injection | |
|---|---|
| Indication | De Quervain Tendinopathy |
| Syringe | 1mL |
| Needle | 25G 16mm |
| Steroid | 0.5mL 20mg triamcinolone |
| Local | 0.5mL 1% lidocaine |
| Volume | 1mL |
Background
Injection for De Quervain Tendinopathy.
Anatomy
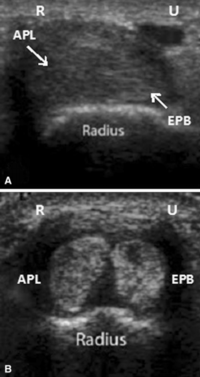
- The APL and EPB usually run together in the first dorsal compartment.
- The tendons can often be seen with the thumb held in resisted extension.
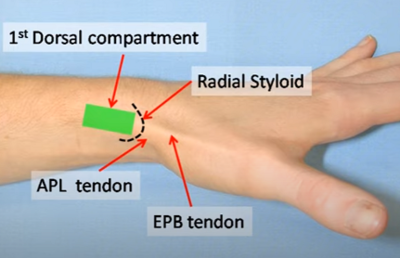
- They can also be palpated at the base of the 1st metacarpal.
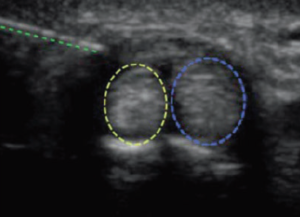
- Anatomic variation: septum with two sub compartments (24-76% in cadaver studies). Failure can occur if failure to inject into compartment or only one sub compartment.
Indications
Contraindications
Technique
- Ultrasound guided is preferred with greater clinical improvement, and allows the identification of subcompartment anatomical variation [2][3][4]
- Position: Ulnar side of hand resting on surface with thumbheld in slight flexion
Non-Ultrasound Guided
- Identify: Radial styloid, the APB and EPL tendons, and the gap between them.
- Injection site
- Usual site: is between 5-10mm proximal to the tip of the radial styloid, between the two tendons, through the retinaculum, within the sheath.
- Alternative site in very thin patients: inject distal to the retinaculum, 5mm distal to the radial styloid (due to limited subcutaneous tissue), then advance the needle proximally while injecting
- Insert needle perpendicularly into the gap then slide proximally between the tendons (needle going distal to proximal)
- Inject solution as a bolus
Ultrasound Guided
- Preparation: Stand off gel recommended
- Identify: APL and APB tendons in sagittal, retinaculum, radial styloid in transverse
- Optional: initial infiltration of lidocaine.
- Axis: Can be done long axis or short axis. Transverse view is best with the needle entering the sheath while in plan with the transducer.
- Direction: Dorsal to palmar direction, at a site free of superficial veins and the superficial branch of the radial nerve
- Injection
- One sheath: deposit at one location in the sheath
- Two sheaths: Pierce the septum between the sheaths. Deposit half around the APL, then draw back and deposit the remaining half around the EPB
Complications
- Subcutaneous fat atrophy, particularly noticeable in dark skinned thin women. This may be permanent but generally resolves within 3 months. The risk can be reduced by using hydrocortisone.
- Trauma to superficial radial nerve
Aftercare
Rest hand for one week with taping. Avoid provoking activities and start a graded load programme.
External Resources
References
- ↑ McDermott JD, Ilyas AM, Nazarian LN, Leinberry CF. Ultrasound-guided injections for de Quervain's tenosynovitis. Clin Orthop Relat Res. 2012;470(7):1925-1931. doi:10.1007/s11999-012-2369-5
- ↑ McDermott JD, Ilyas AM, Nazarian LN, et al. Ultrasound-guided injections for de Quervain's tenosynovitis. Clin Orthop Relat Res. 2012;470:1925–31.
- ↑ Jeyapalan K, Choudhary S. Ultrasound-guided injection of triamcinolone and bupivacaine in the management of de Quervain’s disease. Skelet Radiol. 2009;38:1099–103.
- ↑ Zingas C, Failla JM, Van Holsbeeck M. Injection accuracy and clinical relief of de Quervain’s tendinitis. J Hand Surg Am. 1998;23:89
Literature Review
- Reviews from the last 7 years: review articles, free review articles, systematic reviews, meta-analyses, NCBI Bookshelf
- Articles from all years: PubMed search, Google Scholar search.
- TRIP Database: clinical publications about evidence-based medicine.
- Other Wikis: Radiopaedia, Wikipedia Search, Wikipedia I Feel Lucky, Orthobullets,