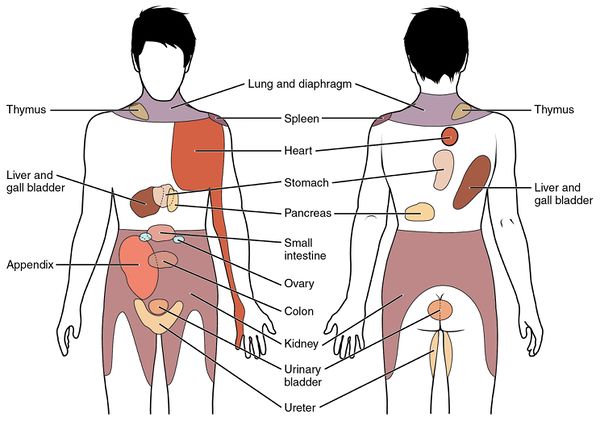
Visceral Pain
Viscero-visceral and viscero-somatic convergence are important clinical concepts. Treatment of one condition may improve symptoms of another when linked through segmental innervation. The resolution of a visceral disease may not resolve the somatic manifestations. Visceral pain manifests some of the same mechanisms seen in somatic pain, but there are crucial differences in central nociceptive processing. Visceral pain also has a strong affective component and can be reinforced by anxiety and depression.[1]
Visceral Innervation
Vagal afferents convey predominantly physiological information, while spinal afferents convey noxious stimuli. There are likely to be three types of nociceptive sensory receptors: High threshold noxious, Low threshold innocuous to noxious, while some are silent and recruited by tissue injury and inflammation. All can be sensitized, and drive central sensitisation that can persist even after the initial insult has resolved. Damage and inflammation also affects normal motility and secretion, producing changes to the nociceptor environment. While ascending pathways include the spinothalamic tract, the dorsal column is more important in nociceptive transmission. Ascending tracts synapse at the thalamus, limbic centres, and the somatosensory cortex. There is no somatotropic representation in the cortex. Pain is represented in the secondary somatosensory cortex. Visceral pain elicits nausea and hypotension, the opposite to somatic pain.
Peripheral sensitisation can occur, but the mechanisms differ from cutaneous sensitisation. Functional visceral disturbance can persist even after the initial insult has resolved. While with central sensitisation, NMDA receptors are likely to play significant role.
Clinical Characteristics
Visceral pain is initially described as vague, central sensation felt anterior or posterior, accompanied by various autonomic and neurovegetative symptoms such as malaise, nausea, sweating, palour, anxiety, changes in blood pressure and heart rate, and sense of impending doom (‘true visceral pain’). Eventually this subsides, and is followed by a variety of symptoms and signs perceived in somatic areas receiving the same innervation. Skin, subcutis and muscle are all involved. Initially, the symptoms of pain rather than pain itself is felt. As time progresses, signs start to develop. The muscle layer is earliest and most commonly involved layer. However, the skin and subcutaneous layers are also commonly involved with hyperalgesia, and sudomotor signs. These symptoms and signs can persist even when the visceral insult has resolved. These symptoms and signs may also, in turn, influence visceral symptoms.
| Symptoms & Signs | Neurobiology |
|---|---|
| Not evoked from all viscera | Not all viscera are innervated by sensory receptors. |
| Not linked to injury | Functional properties of visceral sensory afferents |
| Referred to body wall | Viscerosomatic convergence in central pain pathways |
| Diffuse and poorly localised | Few sensory visceral afferents. Extensive divergence in central nervous system |
| Intense motor and autonomic reactions | Mainly a warning system, with substantial capacity for amplification |
Pain is not evoked from all viscera
It is generally evoked from the liver, kidney, lung parenchyma, and most solid viscera. These features are due to the functional properties of the peripheral receptors of the nerves that innervate certain visceral organs and to the fact that many viscera are innervated by receptors that do not evoke conscious perception and, thus, are not sensory receptors in the strict sense
Pain is not linked to injury
Cutting the intestine causes no pain. But stretching it does (without injury). Pain can be produced by ischaemia, inflammation of the lining of the hollow viscus, stimulation (chemical or mechanical) of inflamed mucous membranes, traction compression or twisting of the mesentery, organ ligaments or blood vessels, or necrosis of the viscera such as the pancreas or myocardium.
Visceral pain is referred to the body wall
Viscero-somatic convergance and referred pain, muscle spasm, and hyperalgesia. All viscera are innervated by thoracolumbar outflow of sympathetic nervous system T1 - L2 via cardiac and splanchnic nerves, with cell bodies in the dorsal root ganglion. During development, viscera change position, drawing their innervation with them. This leads to a mismatching of intra abdominal position and segmental innervation, and enables understanding of pain referral patterns. Visceral sensations are mediated through convergent signals via somatosensory pathways.
Visceral afferents and cutaneous nociceptors converge on similar neurons at some point in the sensory pathways probably at a spinal level, but could occur at thalamic and cortical levels. The resulting impulses may be then misinterpreted at a spinal level as originating in the skin or other somatic structure. Most second order neurons receiving visceral input in laminae I and V, some in ventral horn. Fewest in the superficial dorsal horn. Most in the deep dorsal and ventral horn. Here they have diffuse and bilateral visceral and somatic input, are subject to descending excitatory and inhibitory control. Visceral afferents comprise fewer than 10% of all spinal afferent input. Therefore, visceral sensations can be mediated only through convergent signals via somatosensory pathways.
| Structure | Segmental Innervation | Possible Pain Locations |
|---|---|---|
| Uterus (including uterine ligament) | T1-L1, S2-S4 | LS junction, TL |
| Ovaries | T10-11 | Low abdominal |
| Testes | T10-11 | Sacral |
| Kidney | T10-L1 | LS (ipsi), lower and upper abdominal |
| Ureter | T11-L2, S2-S4 | Groin, upper abdominal, suprapubic, medial, proximal thigh, TL |
| Bladder | T11-L2, S2-S4 | Sacral apex, suprapubic, TL |
| Prostate | T11-L1, S2-S4 | - |
| Oesophagus | T4-6 | Substernal and upper abdominal |
| Stomach | T6-10 | Upper abdominal, middle and lower TS |
| Small Intestine | T7-10 | Middle TS |
| Pancreas | T10 | Upper abdominal, lower TS, upper LS |
| Gallbladder | T7-9 | RUQ, right middle and lower TS, aspect scapula |
| Liver | T7-9 | Upper abdominal, middle TS |
| Common Bile Duct | T8-10 | Lower abdominal, middle TS |
| Large Intestine | T11-L1 | Upper sacral, suprapubic, LLQ |
| Sigmoid Colon | T11-12 | |
| Heart | T1-5 | Cervical anterior, upper thorax, left or right upper extremities. |
| Lungs and Bronchi | T5-6 | TS (ipsi), Cervical (diaphragm involved) |
| Diaphragm (central portion) | C3-5 | CS |
- Viscero-somatic convergence, the visceral somatic reflex (muscle spasm)
may persist long after resolution of visceral insult. Local Rx of muscle hyperalgesia may reduce visceral symptoms.
- Viscero-somatic convergence, cutaneous hyperalgesia
Sensitisation
Visceral pain is diffuse and poorly localised
Due to low density of sensory innervation, and extensive divergence of visceral input within CNS. Low proportion of visceral afferent fibres compared to somatic origin. A few visceral afferents can activate many neurons in the spinal cord. Viscerovisceral convergance contributes to difficulty in pinpointing source of pain. There is also poor representation in the primary somatosensory cortex.
- Viscerovisceral Hyperalgesia
This can occur in patients presenting with more than one painful visceral condition at a time. Occurs if affected organs have share segmental innervation. These include the heart and gallbladder (T5), the uterus and upper urinary tract (T10-L1), the uterus and colon (T10-L1), and the bladder and sigmoid colon/rectum (L1-L2). Enhancement of typical symptoms from all affected viscera, as well as referred phenomenon. Effective treatment of one visceral disease may relieve symptoms from the other disease. Treatment of muscle hyperalgesia may relieve pain of one or both.
- VSR & VVR clinical observations
Effectively treating IHD can ease severity of pain from GB disease and vice versa. Treating dysmennorhoea has been shown to reduce urinary tract pain, pain from IBS, and muscle hyperalgesia. VVH can occur when one condition is ‘silent’ treatment of endometriosis discovered at laparoscopy has reduced urinary symptoms. Effectively treating muscle tenderness can ease pain of dysmennorhoea , IBS and urinary tract.
Visceral pain is associated with intense motor and autonomic reactions
There is the potential for afferent branching to synapse with autonomic efferent fibres. There are both spinal and supraspinal mechanisms.
Naming issues
Many authors fail to appreciate the potential significance of VSC, VSR, VVR. Abdominal wall cutaneous nerve entrapment syndrome, Myofascial pain, Regional pain syndrome, Non specific abdominal wall pain.
Clinical Implications
Neurobiology can help us understand at least some of the basis for MSK pain that may be linked to visceral dysfunction. Numerus studies have demonstrated that manifestations of viscero-somatic convergance can persist after resolution of visceral disease (pain, muscle spasm, hyperalgesia). Hyperalgesia can extend beyond expected segment (diffuse muscle hyperalgesia). Local treatment of muscle hyperalgesia may reduce visceral symptoms. History needs to include assessing current and past visceral symptoms, and timeframe of symptom development. Understanding the VSR can provide insight into the genesis of peripheral symptoms and signs. Awareness of VSR and VVR reminds us that MSK symptomatology should not be treated in isolation, and may involve other disciplines.
VVR can result in increased pain in both viscera, AND muscle hyperalgesia. Effective treatment of one visceral disease can alleviate other spontaneous pain and referred muscle hyperalgesia. VVH can take place when one of the two visceral conditions is latent, or silent.
References
Thank you to Dr Bell for his presentation on the topic.