◒
De Quervain Injection: Difference between revisions
From WikiMSK
| Line 35: | Line 35: | ||
===Ultrasound Guided=== | ===Ultrasound Guided=== | ||
* Identify: APL and APB tendons in sagittal, retinaculum, radial styloid in transverse | * Identify: APL and APB tendons in sagittal, retinaculum, radial styloid in transverse | ||
* Planes | |||
** Out of plane: probe transverse, proximal to distal | |||
** In plane: probe transverse, insert needle from volar to dorsal direction. | |||
==Complications== | ==Complications== | ||
Revision as of 19:13, 30 June 2020
This article is still missing information.
| De Quervain Injection | |
|---|---|
| Indication | De Quervain Tendinopathy |
| Syringe | 1mL |
| Needle | 25G 16mm |
| Steroid | 10-20mg triamcinolone |
| Local | 0.75mL 2% lidocaine |
| Volume | 1mL |
Background
Injection for De Quervain Tendinopathy.
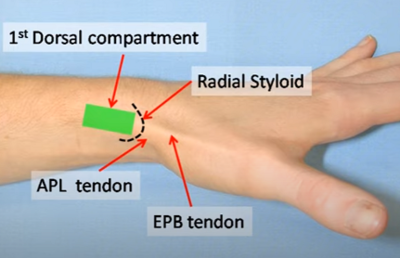
Anatomy
The APL and EPB usually run together in the first dorsal compartment. The tendons can often be seen with the thumb held in resisted extension. They can also be palpated at the base of the 1st metacarpal.
Indications
Contraindications
Technique
- Position: Ulnar side of hand resting on surface with thumbheld in slight flexion
Non-Ultrasound Guided
- Identify: Radial styloid, the APB and EPL tendons, and the gap between them.
- Injection site
- Usual site: is between 5-10mm proximal to the tip of the radial styloid, between the two tendons, through the retinaculum, within the sheath.
- Alternative site in very thin patients: inject distal to the retinaculum, 5mm distal to the radial styloid (due to limited subcutaneous tissue), then advance the needle proximally while injecting
- Insert needle perpendicularly into the gap then slide proximally between the tendons (needle going distal to proximal)
- Inject solution as a bolus
Ultrasound Guided
- Identify: APL and APB tendons in sagittal, retinaculum, radial styloid in transverse
- Planes
- Out of plane: probe transverse, proximal to distal
- In plane: probe transverse, insert needle from volar to dorsal direction.
Complications
- Subcutaneous fat atrophy, particularly noticeable in dark skinned thin women. This may be permanent but generally resolves within 3 months. The risk can be reduced by using hydrocortisone.
- Trauma to superficial radial nerve
Aftercare
Rest hand for one week with taping. Avoid provoking activities and start a graded load programme.