Dynamic Neuromuscular Stabilisation Examination
Several tests are used to assess a variety of parameters under the DNS concept:
- Compare individual postural locomotor patterns with developmental patterns
- Functional centration of individual segments with the ability to maintain individual body segments in a neutral centred position
- Evaluation of dynamic postural trunk stabilisation and muscle coordination responsible for stabilisation of the entire core
- Quality of spinal stabilisation of the spine, chest, and pelvis
- Dual role of the diaphragm in stabilisation and respiratory function
- Distribution of activation between superficial and deep stabilising muscles
- Symmetry and timing of activation of the spinal stabilisation muscles
- Adequacy of muscle activity under load
- Muscle compensatory mechanisms
- Spread of muscle activity to other segments of the body
Diaphragm Test
This is called the diaphragm test. The diaphragm is a respiratory, postural, and sphincter muscle.
- For respiratory function you assess the lateral excursion of the lower ribs during deep inspiration.
- For postural function you evaluate the increase intraabdominal pressure following full exhalation.
- You also evaluate combined respiratory and postural function by assessing breathing while maintaining a slightly raised intra-abdominal pressure.
Assessment of respiratory function:
Position: The patient sits on an examination table, the thighs are supported by hanging freely with the hands relaxed.
Observe from the front: Ask the patient to breath normally while monitoring from the front the quality of the breathing, observing the movement of the ribs, the chest as a whole, the shoulder blades, and the spine.
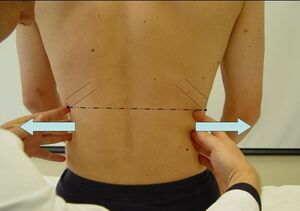
Palpate from behind: Then go behind the patient, and place your fingers along the lower intercostal spaces bilaterally. Slightly press against the lateral group of abdominal muscles. Feel for the position and movement of the lower ribs and assess for Quality and Symmetry of activation.
Correct stereotype: When inspiratory function is normal, the lower ribs move laterally, and the lower intercostal spaces widen, which is directly related to diaphragmatic flattening. Chest and shoulder blades should not move cranially. The spine should be upright.
Incorrect stereotype: When respiration is dysfunctional there is activation of the accessory muscles of respiration, especially sternocleidomastoid, scalenes, pectoralis, and upper trapezius muscles. There is minimal expansion of the lower ribs under the therapists fingers, and the clavicles and scapulae are elevated. With each inhalation the patients chest and shoulders move cranially, the clavicles are horizontal. In combination with a lack of lateral expansion of the lower ribs, there is a pathological synkinesis of the spine. Asymmetry is often observed, with abnormal excursion of the lower ribs more prominent on one side.
Then ask the patient to take a deep breath. With optimal function the diaphragm descends caudally, the lower intercostal spaces widen with intercostal muscle activity, the abdominal wall expands proportionally in all directions.
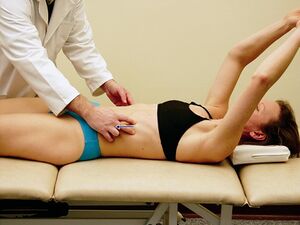
Assessment of postural function: Next palpate dorsolaterally below the ribs at the trigonum lumbale. Palpate to examine the postural function of the diaphragm, feeling for the ability of the diaphragm to lower and expand to its full extent and regulate intra-abdominal pressure.
Ask the patient to push your fingers away. Evaluate the quality of symmetry and effectiveness of expansion of the abdominal wall. The pressure corresponds to the postural function of the diaphragm. With optimal performance, the diaphragm coordinates with the pelvic floor and abdominal wall muscles.
Palpate from the front the area above the inguinal region with your thumbs. Assess the quality and symmetry of intra-abdominal pressure activation. With optimal trunk stabilisation there is concentric activation of the coordinated abdominal wall. Ask the patient to push your fingers away. In dysfunctional activation, the upper part of the rectus abdominis dominates pulling the umbilicus cranially.
Next assess combined respiratory and postural function. From behind, placing your fingers in the lower intercostal spaces, ask the patient to push into your fingers while breathing.
Hip Flexion Test
Here the therapist examines the coordination of the diaphragm, abdominal muscles, and pelvic floor. The patient is seated with legs hanging over the edge of the examination table. The therapist places their hands on the patients back as per the picture to assess for motion. The patient is then asked to lift their ipsilateral knee.
Correct stereotype: The patient should be able to stabilise the thoracolumbar junction and the lumbar spine via regulation of intra-abdominal pressure. This provides a punctum fixum for the iliopsoas muscle.
The thoracic spine should be straight and the thoracolumbar junction stabilised with no lateral shift, no kyphosis, and no lordosis. There should be activation of the laterodorsal part of the abdominal wall.
Poor stereotype: Hyperactivation of the paravertebral muscles (thoracolumbar junction), instability of the thoracolumbar junction with lateral shift towards the side of the lifted knee, trunk lateral flexion to the opposite side, no or weak activation of the latissimus dorsi group of abdominals, hyperactivity of the upper part of rectus abdominus.
Intra-abdominal Pressure Test
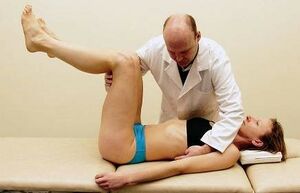
Intra-abdominal pressure regulation is assessed in the supine position. Developmental age is 3 months.
Position: Place the patient in a supine position with the hips and knees at approximately 90 degrees of flexion (triple flexion). The knees should be abducted to the width of the pelvis. Hip abduction corresponds to the width of the shoulders, with slight external rotation at the hips. Support the patients feet.
While slowly releasing support ask the patient to maintain their legs in that position. Check if the patient is able to keep their legs in the air while maintaining their spine in a static position.
Correct stereotype: Raising the legs in the air should increase intra-abdominal pressure enough to stimulate coordinated activity between the anterior and posterior trunk muscles. Under this load the spine, chest, and pelvis should remain in a neutral relaxed position. There is co-contraction of the diaphragm, abdominal muscles, and pelvic floor.
Ask the patient to straighten and bend their lower limbs symmetrically. With ideal stabilising, the hip flexors have a stable fixed point to act through, and the trunk is stable.
Poor stereotype: With dysfunctional activation there is excessive activation of the superficial paraspinal muscles, and there is an increase in lumbar lordosis. By inspection and palpation there is a lack of activation of the lateral abdominal wall and the area above the inguinal region. There is unbalanced activation of the abdominal wall, typically manifesting as a dominance of the upper part of the rectus abdominis and poor activity of the lower abdominal wall. The umbilicus can be pulled cranially and be turned upwards. There may be an abdominal wall diastasis. With an increase in lumbar lordosis, the head may extend along with shoulder protraction and chest elevation.
Another manifestation of poor function is excessive lumbar kyphosis with a posterior pelvic tilt as the patient tries to prevent arching of the lower back. The patient pushes the lower back against the table while over activating rectus abdominis, and extending the head.
Prone Extension Test
This is the trunk and head extension test. It can be performed with or without symmetrical arm support.
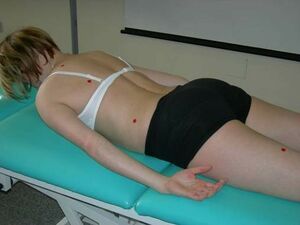
Position: Without arm support the patient is prone, and the upper limbs are relaxed along the body. Ask the patient to lift their head and trunk above the table, slightly extending the spine.
Correct stereotype: With optimal function the pelvis remains neutral on the table, and there is smooth extension of the entire spine. The segment starts at T4 as the punctum fixum. There is balanced activity of the entire abdominal wall and appropriate intra-abdominal pressure regulation. When inspecting from above, the lateral abdominal walls are straight, with a line connecting the ribs to the pelvis. There is appropriate activity of the spine extensors. The scapulae remain in a neutral position connecting to the posterior chest.
Poor stereotype: With dysfunctional activity, spinal extension is not smooth, and the pelvis tilts anteriorly. The trunk remains on the mat, and extension occurs mainly in the cervical and lumbar spine with. The superficial paravertebral spinal muscles are overactive. There is minimal activity of the lateral abdominal wall with convex bulging observed from above. The transversus abdominis aponeurosis becomes concave inwards. There is excessive activity of the hamstring muscles, and occasionally activity of the calf muscles. There may be poor coactivation of deep neck flexors and extensors with neck hyperextension. There may be overactivation of the upper scapula fixator muscles, and decentration of the shoulder girdle. The scapulae may abduct (lower angles), elevate, and externally rotate.
Standing Extension Test
This is the trunk and head extension test. Ask the patient to stand and extend backwards.
Correct stereotype: Check for smooth movement and coordination of the anterior and posterior trunk muscles.
Poor stereotype: In dysfunctional activity there is anterior pelvic tilt, cervical and lumbar hyperextension, and poor thoracic spine extension. The knees may flex.
Quadruped Position
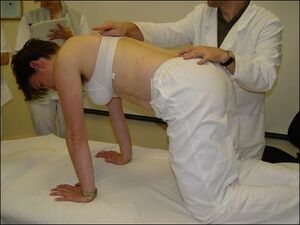
This is the quadruped test on all fours. Developmental age is 7-9 months.
Position: The patient uses hands and knees for support. The knees are approximately the width of the pelvis. The thighs and arms are perpendicular to the ground. Ask the patient to slowly rock back and forth.
Correct stereotype: Observing from the side, spinal alignment should not change during movement, with movement occurring mostly in the shoulders and hips. Observing from above the scapulae should be in a neutral position connecting to the chest. The head should be align with the spine, with a neutral pelvic position, and straight spine. There should be balanced activity of all trunk muscles. Look for centration and muscle coordination of arms and legs. Hand support should be balanced.
Poor stereotype: In insufficient stabilisation there is collapse in the sagittal plane. The spine is not maintained in neutral during rocking. There are several manifestations.
- Lumbar hyperlordosis with an anterior pelvic tilt, and a cervical hyperlordosis with a posterior head tilt.
- Increased lumbar lordosis with thoracic hyperkyphosis. This is associated with neck flexion. As the body moves backwards there may be an increase in lumbar kyphosis.
- Reversal of the curve with thoracic lordosis and scapula adduction. If the scapulae are poorly stabilised the move in different positions. There is decentration of the shoulders with them protracted and internally rotated, the elbow joints hyperextend, and the hand support is on the ulnar aspect.
- Increased thoracic kyphosis with scapula abduction and external rotation of the scapulae tips. There is decentration of the lower upper limb joints with elbow flexion. In the lower extremities, anterior pelvic tilt is associated with internal hip rotation, and overloading of the lateral knees with knee adduction. Increased hamstring activity is due to efforts to maintain the pelvis in neutral. The shins lift with collapse of the pelvis. There may be hyperactivity of the paraspinal extensors, and poor activity of the abdominal muscles observing in the trigonum lumbale and above the inguinal region. There is hyperactivity of the upper trapezius and upper pectoralis major muscles, which manifests as elevation of the scapulae and internal shoulder joint rotation.
Supine Arm Elevation Test
Position: The patient lies supine with their arms by their sides. Ask the patient to smoothly raise their arms in the sagittal plane.
Correct stereotype: During elevation the movement should be smooth occurring in centrated shoulder joints. The chest should be neutral, and the lower ribs should be fixed i.e. not pulled cranially during flexion at the shoulders. The thoracolumbar junction should be stabilised. Up to 120 degrees of elevation the movement is should occur purely in the glenohumeral joint. From 120 to 180 degrees there is contribution from rotation of the scapula tip and extension of the thoracic spine.
Poor stereotype: With dysfunctional activity there is an early cranial shift of the chest, pronounced lumbar lordosis (instability of the thoracolumbar junction), and protraction and elevation of the shoulder girdle, with thoracic hyper-kyphosis. The scapulae loses its stability during movement, resulting in early external rotation of the lower angle, and internal rotation of the glenohumeral joints. This can be observed by witnessing a decrease in distance between the head and arms. Smaller distances correspond to increasing decentration and glenohumeral joint elevation.
The test can also be performed in standing. In dysfunctional activity there is increased lumbar lordosis.
Squat Test
The patient performs a squat slowly to a 90 degree angle, maintaining this position. The arms are held in front to help with balance. The feet are positioned to the width of the pelvis. Developmental age 12 months.
Correct stereotype: Inspection from the side, observe the axis of the trunk and legs which should move in parallel. Ideal movement starts with hip flexion, the knees are stable above the forefeet, and the torso is in neutral with no visible decentration in the sagittal plane. Then inspect from behind. The spine should be in an upright posture with the head in neutral. Palpate the laterodorsal abdominal wall to assess intra-abdominal pressure regulation. From the front there should be joint centration and good three point loading on the feet.
Poor stereotype: In poor stabilisation, there is a loss of the parallel position of the trunk and legs, and there is compromised timing of triple flexion of the leg joints. One example is the knees driving the squat movement, with the knees moving forward of the toes, the weight is on the forefoot, and the trunk is held too vertically. Another pattern is the knees move behind the toe axis, the weight is on the heels, and the toes lift off the floor, and the torso flexes too far forward. In both of these cases, inspection from behind you can observe exaggerated spinal lordosis or kyphosis with a forward head position. The spinal extensors are overactive, and there is insufficient activation palpable at the laterodorsal abdominal wall. There is often asymmetry of pelvic movement, and a shift to one side. From the front there is often decentration of the leg joints. For example internal rotation of the femurs, with medial collapse of the knees, and foot pronation. Also frequent is overload of the lateral aspects of the feet.