Ganglion Impar Injection: Difference between revisions
From WikiMSK
No edit summary |
No edit summary |
||
| Line 18: | Line 18: | ||
==Technique== | ==Technique== | ||
The optimum technique uses a combination of ultrasound and fluoroscopy. Ultrasound alone cannot accurately assess needle depth, while fluroscopy alone cannot accurately identify the sacrococcygeal junction nor its angulation due to bowel gas. The needle is first inserted under ultrasound guidance, and then the depth verified by fluoroscopy. | |||
===Ultrasound Guided=== | ===Ultrasound Guided=== | ||
Ultrasound guided techniques have been described such as by Ghai et Al<ref>{{#pmid:31007658}}</ref> | |||
*Position: prone, lower limbs internally rotated, toes pointing to the opposite foot. This helps to separate the buttocks and provides a flatter sacral hiatus site. | |||
*Place the transducer in the transverse position and visualise the sacral hiatus, the two sacral cornuae, and the sacrococcygeal ligament which traverses the sacral hiatus above the epidural space | |||
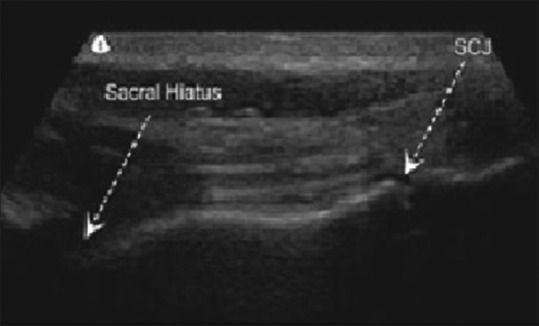
*Obtain a longitudinal position of the sacral hiatus, the proximal portion of the transducer resting between the two cranial sacral cornuae. The first cleft caudal to the sacral hiatus is the sacrococcygeal junction. | |||
*Confirm the location of the sacrococcygeal junction by pressing with a long forceps under sonographic monitoring. | |||
*Anaesthetised the overlying skin | |||
*Advance a 23 gauge needle through the sacrococcygeal junction using an out of plane technique. | |||
*Advance the needle until a loss of resistance is felt, which indicates that the needle tip is ventral to the sacrococcygeal ligament. Note that this is not always felt, hence the ideal use of combined imaging with fluoroscopy to confirm needle depth. Ultrasound cannot visualise the ventral coccyx | |||
*Inject 3-5mL of 1% lidocaine or 10mL of 0.25% bupivicaine and 40mg of methylprednisolone. | |||
===Fluoroscopic Guidance=== | |||
===Non-ultrasound Guided=== | ===Non-ultrasound Guided=== | ||
This is not recommended | |||
==Complications== | ==Complications== | ||
Revision as of 17:36, 26 July 2020
| Ganglion Impar Injection | |
|---|---|
| Indication | |
Background
Anatomy
Indications
Contraindications
Technique
The optimum technique uses a combination of ultrasound and fluoroscopy. Ultrasound alone cannot accurately assess needle depth, while fluroscopy alone cannot accurately identify the sacrococcygeal junction nor its angulation due to bowel gas. The needle is first inserted under ultrasound guidance, and then the depth verified by fluoroscopy.
Ultrasound Guided
Ultrasound guided techniques have been described such as by Ghai et Al[1]
- Position: prone, lower limbs internally rotated, toes pointing to the opposite foot. This helps to separate the buttocks and provides a flatter sacral hiatus site.
- Place the transducer in the transverse position and visualise the sacral hiatus, the two sacral cornuae, and the sacrococcygeal ligament which traverses the sacral hiatus above the epidural space
- Obtain a longitudinal position of the sacral hiatus, the proximal portion of the transducer resting between the two cranial sacral cornuae. The first cleft caudal to the sacral hiatus is the sacrococcygeal junction.
- Confirm the location of the sacrococcygeal junction by pressing with a long forceps under sonographic monitoring.
- Anaesthetised the overlying skin
- Advance a 23 gauge needle through the sacrococcygeal junction using an out of plane technique.
- Advance the needle until a loss of resistance is felt, which indicates that the needle tip is ventral to the sacrococcygeal ligament. Note that this is not always felt, hence the ideal use of combined imaging with fluoroscopy to confirm needle depth. Ultrasound cannot visualise the ventral coccyx
- Inject 3-5mL of 1% lidocaine or 10mL of 0.25% bupivicaine and 40mg of methylprednisolone.
Fluoroscopic Guidance
Non-ultrasound Guided
This is not recommended