Plica Syndrome: Difference between revisions
No edit summary |
No edit summary |
||
| Line 11: | Line 11: | ||
|treatment=Activity modification, analgesia, corticosteroid injection | |treatment=Activity modification, analgesia, corticosteroid injection | ||
}} | }} | ||
'''Plica Syndrome''' is a painful knee condition due to a pathological synovial plica. | '''Plica Syndrome''' is a painful knee condition due to a pathological synovial plica. The medial plica is the most commonly symptomatic. | ||
== Anatomy == | == Anatomy == | ||
The plicae are embryonic remnants of the normal joint compartment separations that fold inwards and are present in most knees. They are normally a thin (almost transparent), vascular, and pliable band of tissue. They originate from the synovial lining and cross the [[Synovial Joint|synovial joint]]. | The plicae are embryonic remnants of the normal joint compartment separations that fold inwards and are present in most knees. They are normally a thin (almost transparent), vascular, and pliable band of tissue. They originate from the synovial lining and cross the [[Synovial Joint|synovial joint]]. | ||
The plicae are indirectly attached to the quadriceps and fat pad. | |||
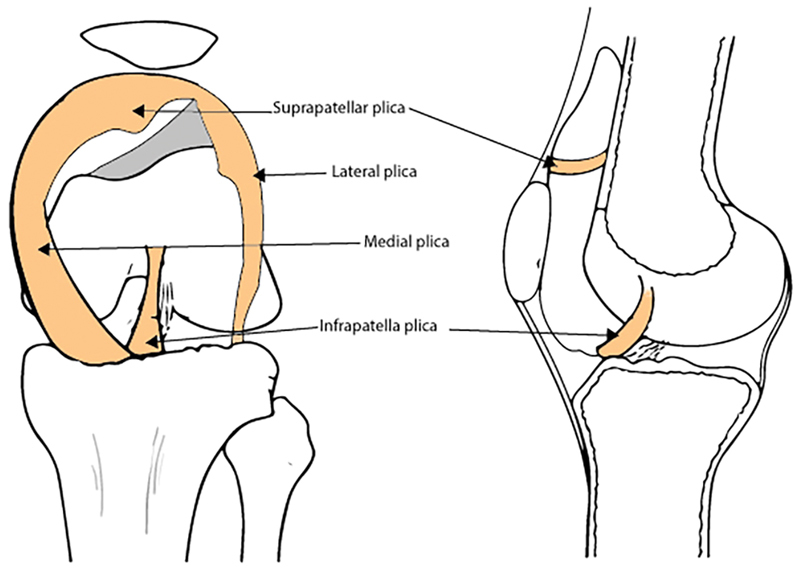
Plicae can be found int he suprapatellar, medial, infrapatellar, or lateral compartments of the [[Knee Joint|knee]] | Plicae can be found int he suprapatellar, medial, infrapatellar, or lateral compartments of the [[Knee Joint|knee]] | ||
==Pathophysiology== | ==Pathophysiology== | ||
A plica can become pathological | A plica can become pathological through an inflammatory process. This can occur from direct blunt trauma, repetitive injury, or from irritation from another knee abnormality such as osteochondritis dissecans or inflammatory arthritis. | ||
This results in it becoming fibrotic, avascular, and inelastic. It can even become hyalinised. This taut nonpliable band can rub or bowstring over the medial femoral condyle or it can become trapped between the patella and femoral condyle causing impingement. | |||
The medial plica is most commonly symptomatic. | The medial plica is most commonly symptomatic. | ||
==Clinical Features== | ==Clinical Features== | ||
[[File:Knee plica inspection.mp4|thumb|Visible clicking on knee inspection.]] | |||
The clinical features are often identical to other intra-articular knee pathologies. | |||
=== History === | |||
The symptoms are usually nonspecific anterior or anteromedial knee pain (parapatellar), often following direct trauma or a repetitive injury. | |||
On examination for medial plica syndrome there may be slight swelling medial to the patellar margin. | The pain is often worse with sitting for long periods (called the theatre sign) or after sleeping. It is also often worse with squatting, kneeling, or walking upstairs. ' | ||
There may be mechanical symptoms such as clicking, catching, clunking, grinding, giving way, or popping with knee flexion and extension. | |||
=== Examination === | |||
On examination for medial plica syndrome there may be slight swelling medial to the patellar margin. | |||
The plica fold is located around the joint lines in the anterior knee compartment. The plica feel like a ribbon of tissue which can be rolled over the medial femoral condyle. The band of tissue runs either parallel or at a slight oblique angle to the medial border of the patellar. Flexing the knee to 90 degrees may make this easier to palpate. Record any tenderness. | |||
'''Medial patellar plica test''': The patient is supine. Apply pressure over the inferomedial border of the patellofemoral joint. This pushes the plica between the medial patella and medial femoral condyle. Maintain the pressure and passively flex the knee from 0 to 90 degrees. A positive test is provocation of pain at this extended position that is relieved at 90 degrees of flexion. | '''Medial patellar plica test''': The patient is supine. Apply pressure over the inferomedial border of the patellofemoral joint. This pushes the plica between the medial patella and medial femoral condyle. Maintain the pressure and passively flex the knee from 0 to 90 degrees. A positive test is provocation of pain at this extended position that is relieved at 90 degrees of flexion. | ||
A full [[Knee Examination|knee examination]] should also be performed. | |||
==Investigations== | ==Investigations== | ||
Revision as of 17:36, 25 April 2022
Plica Syndrome is a painful knee condition due to a pathological synovial plica. The medial plica is the most commonly symptomatic.
Anatomy
The plicae are embryonic remnants of the normal joint compartment separations that fold inwards and are present in most knees. They are normally a thin (almost transparent), vascular, and pliable band of tissue. They originate from the synovial lining and cross the synovial joint.
The plicae are indirectly attached to the quadriceps and fat pad.
Plicae can be found int he suprapatellar, medial, infrapatellar, or lateral compartments of the knee
Pathophysiology
A plica can become pathological through an inflammatory process. This can occur from direct blunt trauma, repetitive injury, or from irritation from another knee abnormality such as osteochondritis dissecans or inflammatory arthritis.
This results in it becoming fibrotic, avascular, and inelastic. It can even become hyalinised. This taut nonpliable band can rub or bowstring over the medial femoral condyle or it can become trapped between the patella and femoral condyle causing impingement.
The medial plica is most commonly symptomatic.
Clinical Features
The clinical features are often identical to other intra-articular knee pathologies.
History
The symptoms are usually nonspecific anterior or anteromedial knee pain (parapatellar), often following direct trauma or a repetitive injury.
The pain is often worse with sitting for long periods (called the theatre sign) or after sleeping. It is also often worse with squatting, kneeling, or walking upstairs. '
There may be mechanical symptoms such as clicking, catching, clunking, grinding, giving way, or popping with knee flexion and extension.
Examination
On examination for medial plica syndrome there may be slight swelling medial to the patellar margin.
The plica fold is located around the joint lines in the anterior knee compartment. The plica feel like a ribbon of tissue which can be rolled over the medial femoral condyle. The band of tissue runs either parallel or at a slight oblique angle to the medial border of the patellar. Flexing the knee to 90 degrees may make this easier to palpate. Record any tenderness.
Medial patellar plica test: The patient is supine. Apply pressure over the inferomedial border of the patellofemoral joint. This pushes the plica between the medial patella and medial femoral condyle. Maintain the pressure and passively flex the knee from 0 to 90 degrees. A positive test is provocation of pain at this extended position that is relieved at 90 degrees of flexion.
A full knee examination should also be performed.
Investigations
Imaging is poor at visualising this condition. MRI is done sometimes to exclude mimics.
Treatment
Activity modification, analgesia, corticosteroid injection
Further Reading
 Lee et al.. Synovial Plica Syndrome of the Knee: A Commonly Overlooked Cause of Anterior Knee Pain. Surgery journal (New York, N.Y.) 2017. 3:e9-e16. PMID: 28825013. DOI. Full Text.
Lee et al.. Synovial Plica Syndrome of the Knee: A Commonly Overlooked Cause of Anterior Knee Pain. Surgery journal (New York, N.Y.) 2017. 3:e9-e16. PMID: 28825013. DOI. Full Text.
Literature Review
- Reviews from the last 7 years: review articles, free review articles, systematic reviews, meta-analyses, NCBI Bookshelf
- Articles from all years: PubMed search, Google Scholar search.
- TRIP Database: clinical publications about evidence-based medicine.
- Other Wikis: Radiopaedia, Wikipedia Search, Wikipedia I Feel Lucky, Orthobullets,