Caudal Epidural Steroid Injection: Difference between revisions
No edit summary |
No edit summary |
||
| Line 8: | Line 8: | ||
}} | }} | ||
== | ==Background== | ||
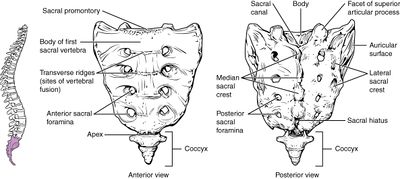
[[File:Sacrum_and_Coccyx.jpg|400px]] | [[File:Sacrum_and_Coccyx.jpg|400px]] | ||
*Thecal sac ends at S2 (PSIS level) | |||
==Technique== | ==Ultrasound Guided Technique== | ||
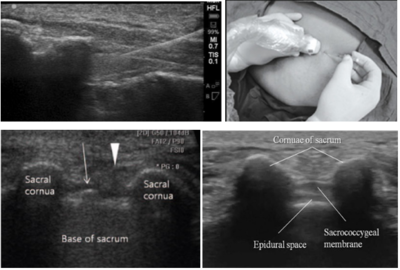
[[File:Caudal Epidural Injection Ultrasound.PNG|400px]] | [[File:Caudal Epidural Injection Ultrasound.PNG|400px]] | ||
| Line 20: | Line 21: | ||
* Terminate needle advancement right after piercing the sacrococcygeal ligament. This is to avoid injection into the venous plexus and intrathecal injection in those with unusually low terminating dural sacs. | * Terminate needle advancement right after piercing the sacrococcygeal ligament. This is to avoid injection into the venous plexus and intrathecal injection in those with unusually low terminating dural sacs. | ||
* Aspirate to ensure needle not penetrated thecal sac or blood vessel. If aspirate CSF then abort procedure and retry in one week. | * Aspirate to ensure needle not penetrated thecal sac or blood vessel. If aspirate CSF then abort procedure and retry in one week. | ||
==Non-Ultrasound Guided Technique== | |||
*Find and mark cornuae | |||
*Infiltrate lidocaine to overlying soft tissue | |||
*Enter at midline, feel it penetrate the membrane, aspirate, slow i.e. over 10 mins inject contents | |||
*Assess post procedure for improvement in provocative manoeuvres such as SLR and pain | |||
*Monitor (IV access?) Empty bladder | |||
==Indications== | ==Indications== | ||
| Line 25: | Line 34: | ||
==Risks== | ==Risks== | ||
Infection, subcutaneous injection, spinal cord infarction, Radiculopathy <1:2,000 paraplegia 1:50,000, allergic reaction, intravascular injection (minimal risks with dexamethasone due to small particulate size), dural puncture with headache, PE, ADR from steroids, increased back pain (3.1%) | Infection, subcutaneous injection, spinal cord infarction, Radiculopathy <1:2,000 paraplegia 1:50,000, allergic reaction, intravascular injection (minimal risks with dexamethasone due to small particulate size), dural puncture with headache, PE, ADR from steroids, increased back pain (3.1%) | ||
==Aftercare== | ==Aftercare== | ||
Advised to keep active within pain limits, and is reassessed about 10 days later. Steroid remains in situ for about 2 weeks. Up to 3-4 injections may be performed before declaring the therapy a failure. Max 0.6mg/kg or 40mg dexamethasone per year. | Monitor for allergy. Advised to keep active within pain limits, and is reassessed about 10 days later. Steroid remains in situ for about 2 weeks. Up to 3-4 injections may be performed before declaring the therapy a failure. Max 0.6mg/kg or 40mg dexamethasone per year. | ||
[[Category:Lumbar Spine]] | [[Category:Lumbar Spine]] | ||
[[Category:Spine Procedures]] | [[Category:Spine Procedures]] | ||
Revision as of 16:14, 30 June 2020
| Caudal Epidural Steroid Injection | |
|---|---|
| Indication | Radicular leg pain |
| Syringe | 20mL |
| Needle | 21G 40mm, or 25G 50mm |
| Steroid | Must be dexamethasone, 15mg |
| Local | No local, add normal saline |
| Volume | L5: 10mL L3: 15mL Upper lumbar: 20mL |
Background
- Thecal sac ends at S2 (PSIS level)
Ultrasound Guided Technique
- Position: prone with heels rotated laterally, and a cushion pillow is used as an iliac wedge.
- Identify sacral cornua at base of imaginary triange with thumb (needle will go between cornua)
- Obtain a transverse image for the sacral hiatus and dorsal sacrococcygeal ligament between the bilateral sacral cornua,
- Obtain a longitudinal view and advance needle at a 45 degree angle.
- Terminate needle advancement right after piercing the sacrococcygeal ligament. This is to avoid injection into the venous plexus and intrathecal injection in those with unusually low terminating dural sacs.
- Aspirate to ensure needle not penetrated thecal sac or blood vessel. If aspirate CSF then abort procedure and retry in one week.
Non-Ultrasound Guided Technique
- Find and mark cornuae
- Infiltrate lidocaine to overlying soft tissue
- Enter at midline, feel it penetrate the membrane, aspirate, slow i.e. over 10 mins inject contents
- Assess post procedure for improvement in provocative manoeuvres such as SLR and pain
- Monitor (IV access?) Empty bladder
Indications
Good evidence for radicular leg pain due to lumbar disc herniation. 72.5% complete or partial pain relief at 12 weeks in those with symptom duration of 4-52 weeks. Fair evidence for axial pain and spinal stenosis and post surgery syndrome
Risks
Infection, subcutaneous injection, spinal cord infarction, Radiculopathy <1:2,000 paraplegia 1:50,000, allergic reaction, intravascular injection (minimal risks with dexamethasone due to small particulate size), dural puncture with headache, PE, ADR from steroids, increased back pain (3.1%)
Aftercare
Monitor for allergy. Advised to keep active within pain limits, and is reassessed about 10 days later. Steroid remains in situ for about 2 weeks. Up to 3-4 injections may be performed before declaring the therapy a failure. Max 0.6mg/kg or 40mg dexamethasone per year.