Hand and Wrist Biomechanics
The wrist connects the hand to the forearm and is key to hand function. The hand allows for complex manipulation of our environment and is the final link in the mechanical chain that begins at the shoulder.
Anatomy
Wrist
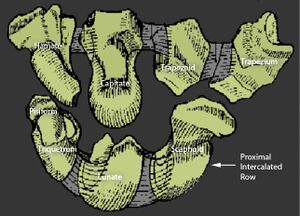
The distal carpal row forms a relatively immobile transverse unit that articulates with the metacarpals to form the carpometacarpal joints. All four bones in the distal row fit tightly against each other and are held together by stout interosseous ligaments.
The more mobile proximal row consists of the scaphoid, lunate, and triquetrum. This row articulates with the distal radius and soft tissue triangular fibrocartilage to form the radiocarpal joint.
The proximal component of the radiocarpal joint is the concave surface of the distal radius and the triangular fibrocartilage (also known as the articular disc). The eighth carpal bone, the pisiform, is a sesamoid bone that mechanically enhances the wrist’s most powerful motor, the flexor carpi ulnaris.
The palmar surface of the carpus as a whole is concave, constituting the floor and walls of the carpal tunnel. The motor branch of the ulnar nerve (not shown) winds around the base of the hook before entering the deep palmar compartment.
Hand
The digital rays are numbered from the radial to the ulnar side: I (thumb), II (index finger), III (middle finger), IV (ring finger), and V (little finger). Each digital ray articulates proximally with a particular carpal bone to form the carpometacarpal (CMC) joint.
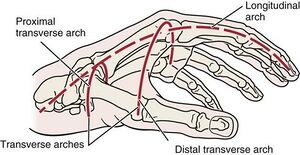
The bones of the hand are arranged in three arches, two transverse and one longitudinal. The proximal transverse arch, with the capitate as its keystone, lies at the level of the distal carpus and is relatively fixed. The distal transverse arch, with the head of the third metacarpal as its keystone, passes through all of the metacarpal heads and is more mobile. The two transverse arches are connected by the rigid portion of the longitudinal arch, which is composed of the four digital rays and the proximal carpus. The second and third metacarpal bones form the central pillar of this arch. The longitudinal arch is completed by the individual digital rays, and the mobility of the thumb and fourth finger and fifth finger rays around the second and third fingers allows the palm to flatten or cup itself to accommodate objects of various sizes and shapes.
The skin on the dorsum or the back of the hand differs and is distinct from the skin that covers the palmar surface. Dorsal skin is mobile, often regarded as very fine, and highly flexible, allowing for a wide array of articular movements. In contrast, palmar skin is thick, glabrous, and inelastic. Palmar skin plays a significant role in hand perceptibility or the perception of touch, safety of the upper limb through sensory protection, and in providing support for the limb during weight-bearing.
Innervation
The wrist and the hand are innervated for motor and sensory function by three peripheral nerves, the radial, median, and ulnar, that descend from the brachial plexus. Motor or sensory impairment correlates to the location of the injury or impingement along a particular nerve tract. The radial nerve primarily innervates those muscles that facilitate extension of the wrist and the digits, namely the long wrist extensors. Impairment to the radial nerve can cause wrist drop and produce wrist instability that impedes hand grasp. In terms of sensory function, the radial nerve supplies the skin along the radial sphere of the forearm and the hand, and sensory impairment in radial nerve denervation minimally impedes hand function.
The median nerve primarily innervates the long wrist and hand extrinsic flexors. Thus, high-level median nerve impairment affects the radial flexor muscles of the hand more greatly than it does the flexor capacity along the ulnar side. The median nerve is most critical to fine motor hand function because of the motor and sensory supply that it provides. The median nerve is often regarded as the eyes of the hand because it is responsible for the innervation of the first three digits of the hand on the palmar surface. Without adequate sensation in these digits, fine motor skill is compromised or lost.
The ulnar nerve is regarded as the hand’s power source for hand grasp. It innervates the muscles along the ulnar sphere, including the ulnar hand flexors and most of the hand intrinsics, particularly those responsible for digital adduction and abduction. The ulnar nerve is known for its ability to protect the upper limb as it innervates the skin surface along the ulnar border. Most resting patterns for the upper limb or hand use are performed with the upper limb positioned so that the ulnar borders of the forearm, wrist, and hand are in direct contact with the environment or giving support to the body by direct and sustained weight-bearing or contact onto a surface. Irritation or compression of the ulnar nerve along its path from the elbow to the wrist may impair hand function.
Stability
Bony mechanisms
In the sagittal plane of the wrist, both the scaphoid and the lunate are wedge shaped with the palmar aspect of both bones being wider than the dorsal aspect.
Wrist ligaments
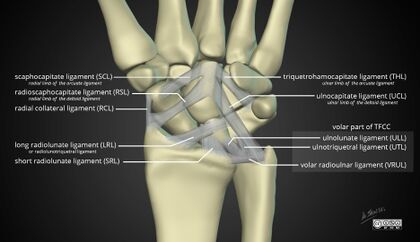
The palmar ligaments are thick and strong, whereas the dorsal ligaments are much thinner and fewer in number. The extrinsic ligaments run from radius to carpus and from carpus to metacarpals. The intrinsic ligaments originate and insert on the carpus. The palmar extrinsic ligaments include the radial collateral ligament, the palmar radiocarpal ligaments, and components of the triangular fibrocartilage complex
(TFCC). The radial collateral ligament is actually more palmar than lateral and is viewed as the most lateral of all palmar radiocarpal fascicles rather than as a collateral ligament per se, because the function of a true collateral ligament is not functionally advantageous in the wrist.
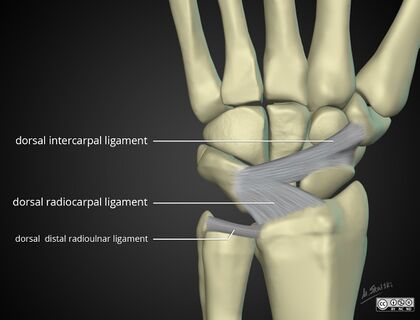
The dorsal extrinsic ligaments include the three bands of the dorsal radiocarpal ligament. Originating from the rim of the radius, these three fascicles insert firmly into the lunate (radiolunate ligament), triquetrum (radiotriquetral ligament), and scaphoid (radioscaphoid ligament), respectively.
The intrinsic ligaments can be grouped into three categories (short, long, and intermediate) according to their length and the relative intercarpal movement they allow. The three short intrinsic ligaments—palmar, dorsal, and interosseous—are stout, unyielding fibers that bind the adjacent carpal bones tightly. These strong ligaments are responsible for maintaining the four bones of the distal carpal row as an
integrated kinematic unit. Three intermediate intrinsic ligaments are located between the lunate and triquetrum, the scaphoid and lunate, and the scaphoid and trapezium. Of the two long intrinsic ligaments—dorsal intercarpal and palmar intercarpal— the palmar is the more important. Also called the deltoid, or V, ligament, it stabilizes the capitate because it attaches to its neck and fans out proximally to insert into the scaphoid and triquetrum. The dorsal intercarpal ligament originates from the triquetrum and courses laterally and obliquely to insert on the scaphoid and trapezium.
| Extrinsic Ligaments | Intrinsic Ligaments |
|---|---|
| Proximal (radiocarpal) | Short |
| —Radio collateral | —Palmar |
| Palmar radiocarpal | —Dorsal |
| —Superficial | Intermediate |
| —Deep | —Lunotriquetral |
| ——Radioscaphocapitate (radiocapitate) | —Scapholunate |
| ——Radiolunate | —Scaphotrapezium |
| ——Radioscapholunate | Long |
| Ulnocarpal complex | —Palmar intercarpal (V, deltoid) |
| ——Meniscus homologue (radiotriquetral) | —Dorsal intercarpal |
| ——Triangular fibrocartilage (articular disc) | - |
| ——Ulnar collateral ligament | - |
| ——Ulnolunate ligament | - |
| —Dorsal radiocarpal
Distal (carpometacarpal) |
- |
TFCC
The components of the TFCC are the meniscus homologue, the triangular fibrocartilage (articular disc), the palmar ulnocarpal ligament (consisting of the ulnolunate and ulnotriquetral ligaments), the ulnar collateral ligament, and the poorly distinguishable dorsal and palmar radioulnar ligaments. The meniscus homologue and the triangular fibrocartilage have a common origin from the dorsoulnar corner (sigmoid notch) of the radius. From there, the meniscus courses toward the palm and around the ulnar border of the wrist to insert firmly into the triquetrum, while the triangular fibrocartilage extends horizontally to insert into the base of the ulnar styloid process. Between the meniscus homologue and the triangular fibrocartilage there is often a triangular area, the prestyloid recess, which is filled with synovium. Dorsally, the TFCC has a weak attachment to the carpus except where some of its fibers join the tendon sheath of the flexor carpi ulnaris dorsolaterally. The ulnolunate ligament connects the palmar border of the triangular fibrocartilage with the lunate. The ulnar collateral ligament arises from the ulnar styloid process and extends distally to the base of the fifth metacarpal bone.
The functions of the TFCC are to stabilize the distal radioulnar joint, reinforce the ulnar aspect of the wrist, form the ulnar aspect of the proximal articulating surface of the radiocarpal joint, and transmit approximately 16% of the compressive forces when the wrist is in the neutral position.
Hand ligaments
All of the digital articulations have one essential feature in common: They are designed to function in flexion. Each joint has firm collateral ligaments bilaterally and a thick anterior capsule reinforced by a fibrocartilaginous structure known as the palmar (volar) plate. By comparison, the dorsal capsule is thin and lax.
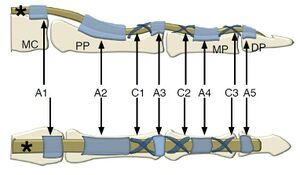
Digital Flexor Tendon Sheath Pulley System
As they extend from their muscles, the digital flexor tendons pass through the carpal tunnel, along with the tendon of the flexor pollicis longus and the median nerve, before fanning out toward their respective digits. The flexor superficialis tendon inserts on the middle phalanx, and the flexor profundus inserts on the distal phalanx. In each digit, these two tendons, surrounded by their synovial sheaths, are held against the phalanges by a fibrous sheath.
At strategic locations along the sheath are five dense annular pulleys (designated as Al, A2, A3, A4, and A5) and three thinner cruciform pulleys (Cl, C2, and C3). These pulleys allow for a smooth curve so that no sharp or angular bends exist in the course of the tendon.
At the point where the A3 pulley traverses the PIP joint, the tension in the tendon generated by joint flexion either pulls the pulley away from its attachment to the bone or pulls the bone away from the joint. This is no problem in a normal, stable joint, but when the joint becomes unstable, as in a patient with rheumatoid arthritis, there could be a danger of severe PIP subluxation.
Digital Collateral Ligaments
A unique feature of the MCP joint is its asymmetry, which is apparent both in the bony configuration of the metacarpal head and in the location of the radial and ulnar collateral ligament attachments to it. The collateral ligaments of the MCP joint extend obliquely forward from the proximal attachment at the dorsolateral aspect of the metacarpal head to their insertion on the palmolateral aspect of the base of the proximal phalanx. The bilateral asymmetry in the site of the attachment of these ligaments manifests itself particularly in the asymmetric range of abduction-adduction in these joints. The asymmetric bilateral arrangement of the interossei also contributes to the overall asymmetry of the MCP joints.
When the MCP joint was flexed from 0º to 80º, the dorsal portion of the ligaments lengthened 3 to 4 mm, the middle portion elongated slightly, and the palmar portion shortened 1 to 2 mm. When the MCP joint moved into hyperextension, the dorsal portion of the ligaments shortened 2 to 3 mm, the middle third shortened slightly, and the palmar third lengthened slightly. Thus, the dorsal portions of both collateral ligaments appear to provide the principal restraining force when the MCP joint is flexed, whereas the palmar portions. provide a restraining force during MCP extension. Therapists will often splint the traumatized or postsurgical MCP joint into 60º to 70º of flexion to place a relative stretch on the collateral ligaments to prevent extension contracture when immobilization is required.
The collateral ligaments are found to be slack when the MCP joints are held positioned in extension and are taut when the MCPs are positioned in flexion. By placing the MCPs into full flexion, the cam configuration of the metacarpal head tightens the collateral ligaments and the lateral mobility or “play” observed when the MCPs are held into extension is limited. The transverse intermetacarpal ligament, which connects the palmar plates, gives additional stability to the MCP region. The extensor tendons are linked to this transverse structure by the transverse laminae, which hold them in position on the dorsal side of the MCP joint.
Volar Plate
In addition to the role of the collateral and accessory collateral ligament, attention is brought to the function of the palmar or volar plate. The accessory collateral ligaments are just palmar to the radial and ulnar collateral ligaments, which originate from the metacarpal and insert into the thick palmar fibrocartilaginous plate. This plate on the volar surface of the MCP is firmly attached to the base of the proximal phalanx, and it is loosely attached to the volar surface of the neck of the metacarpal. This anatomic alignment allows for the volar plate to slide proximally like a moving visor during MCP flexion.
The volar plates are connected by the transverse intermetacarpal ligaments that then connect each plate to its neighbor. They serve to reinforce the joint capsule anteriorly, prevent impingement of the flexor tendons during MCP flexion, and limit hyperextension of the MCP joint.
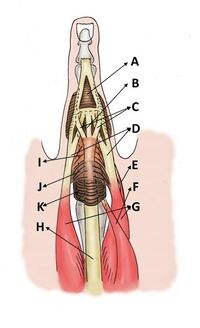
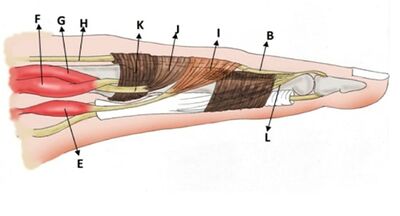
Digital Extensor Assembly System
The long extensor tendons are flat structures that emerge from their synovial sheaths at the dorsal side of the carpus and run over the MCP joint; they are held in this position by the sagittal bands. At the dorsum of the proximal phalanx, these extensor tendons and parts of the interossei interweave so as to form a tendinous complex, the extensor assembly (also known as the extensor mechanism), which extends over both IP joints.
Trifurcation of the long extensor tendon and fanning of interosseous fibers result in the formation of one medial and two lateral bands. The medial band (or central slip) runs dorsally over the trochlea of the proximal phalanx and inserts into the base of the middle phalanx. The two lateral bands course alongside the shoulders of the PIP joint. These bands pursue their way distally and merge over the dorsum of the middle phalanx, forming the terminal tendon, which inserts into the dorsal tubercle of the distal phalanx. This terminal tendon is linked to the proximal phalanx by means of the oblique retinacular ligaments. These ligaments originate from the proximal phalanx and run laterally around the PIP joint, just palmar to the center of motion of this joint in the extended position, to join the terminal tendon.
Muscular Mechanisms of the Wrist and Hand
Except for the flexor carpi ulnaris tendon, which attaches to the pisiform, all of the wrist muscle tendons traverse the carpal bones to insert on the metacarpals.
There are two muscle systems of the hand: extrinsic and intrinsic. The muscle bellies of the extrinsic muscles are primarily located near the elbow with their tendons passing into the hand and into the digital rays. Meanwhile the intrinsic muscle bellies and tendons are entirely found in the hand itself and allow for more powerful motions controlled by the extrinsic muscles as well as providing the ability for more delicate tasks.
Movement
The articulations of the wrist joint complex allow motion in two planes: flexion extension (palmar flexion and dorsiflexion) in the sagittal plane and radial-ulnar deviation (abduction-adduction) in the frontal plane. pronation and supination, results instead from motion arising at the proximal and distal radioulnar and the radiohumeral joints.
Range of Motion
The normal wrist range of motion is 65º to 80º of flexion and 55º to 75º of extension, but it can vary widely among individuals. Owing to a slight palmar tilt of the distal radial plates, flexion exceeds extension by an average of 10º. In a cadaveric study, Kaufmann et al. (2006) found that, in flexion, 75% of wrist motion occurred at the radioscaphoid joint, and 50% occurred at the radiolunate joint, suggesting that the proximal carpal bones do not move as a fixed unit during wrist flexion. In extension, this finding was even more pronounced, with 92% of the wrist motion occurring at the radioscaphoid joint whereas only 52% occurred at the radiolunate joint. Furthermore, the scaphoid and capitate tended to move together, whereas midcarpal motion between the lunate and capitate was evident.
The total arc of radial-ulnar deviation is approximately 50º to 60º, 15º to 20º radialward and 35º to 40º ulnarward. The distal carpal row follows the finger rays during both radial and ulnar deviation, whereas the proximal carpal row glides in the direction opposite to hand movement with greater excursion during ulnar deviation. Radial and ulnar deviation occurs primarily at the midcarpal joint.
Dart Thrower’s Motion
During DTM, the axes of motion for the radiocarpal and midcarpal joints converge, thereby allowing for synergistic motion through a relatively wide arc.
Forearm Pronation & Supination
Average range of motion of pronation-supination is 160º (75º of pronation and 85º of supination). During pronation and supination, the radial head rotates within the fibro-osseous ring formed by the annular ligament and the radial notch of the ulna and spins with respect to the lateral humeral condyle. Distally, the radius glides with respect to the ulna at the distal radioulnar joint. The dorsal and palmar
capsular ligaments of the distal radioulnar joint limit motion at the extremes of pronation and supination, respectively.
Fingers
The second and third metacarpals are linked to the trapezoid and capitate and to each other by tight- fitting joints that are basically immobile. As a result, these metacarpal and carpal bones constitute the “immobile unit” of the hand. The articulations of the fourth and fifth metacarpals with the hamate permit a modest amount of motion: 10º to 15º of flexion-extension at the fourth CMC joint and 20º to 30º at the fifth.
The MCP joints of the four fingers are unicondylar diarthrodial joints, allowing motion in three planes: flexion-extension (sagittal plane), abduction-adduction (frontal plane), and slight pronation-supination (transverse plane), which is coupled with abduction-adduction.
Thumb
At the CMC level, the base of the thumb metacarpal forms a saddle joint with the Trapezium.
Interactions of Wrist and Hand Motions
Wrist extension is synergistic to finger flexion and increases the length of the finger flexor muscles, allowing increased flexion with stretch. Conversely, some flexion of the wrist puts tension on the long
extensors, causing the fingers to open automatically and aiding full finger extension.
Grip strength was greatest at approximately 20º of wrist extension and was least at 40º of wrist flexion.
For grip to be effective and have maximal force, the wrist must be stable and must be in slight extension and ulnar deviation. This conclusion is consistent with the findings concerning load transmission through the ulnar TFCC structures. The position of the wrist also changes the position of the thumb and fingers, thus affecting the ability to grip. When the wrist is flexed with the hand relaxed, the pulp of the thumb reaches only the level of the DIP of the index finger; with the wrist extended, the pulps of the thumb and index finger are passively in contact, creating an optimal situation for gripping or pinching.
The hook grasp is the only grasp pattern available when the hand intrinsics are not working.
Summary
- Motions at the wrist include flexion-extension and radial-ulnar deviation. Stability during radial-ulnar deviation is provided by a double-V system formed by the palmar intrinsic ligament and the radiolunate and ulnolunate ligaments.
- The dart thrower’s motion, the arc from radial extension to ulnar flexion, is a functional movement arc throughout which the proximal carpal row forms a stable base for powerful grip and fine motor control tasks.
- The flexor carpi ulnaris is the most powerful wrist motor and tends to place the wrist in a position of flexion and ulnar deviation.
- The components of the digital extensor assembly, especially the oblique retinacular ligaments, account for the release of the distal phalanx and the coupling of PIP and DIP joint motion.
- A unique feature of the MCP joints is their asymmetry, reflected in the bony configuration of the metacarpal heads, in the attachments of the collateral ligaments, and in the arrangement of the interossei.
- The MCP joints are stabilized primarily by the radial and ulnar collateral ligaments and also by the transverse intermetacarpal ligament, which links the palmar plates to each other.
References
Nordin, Margareta, and Victor H. Frankel. Basic biomechanics of the musculoskeletal system. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins, 2012.
- ↑ Ditsios K, Konstantinou P, Pinto I, Karavelis A, Kostretzis L (2017) Extensor Mechanism’s Anatomy at the Metacarpophalangeal Joint. MOJ Orthop Rheumatol 8(4): 00319. DOI: 10.15406/mojor.2017.08.00319