Lumbar Disc Precision Treatment: Difference between revisions
(→Fusion) |
(→Fusion) |
||
| Line 7: | Line 7: | ||
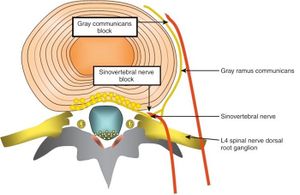
Sinuvertebral nerves, formed by a somatic root from ventral ramus and an autonomic root from grey ramus communicans. An ascending branch passes as far as the above vertebral disc. A descending branch supplies the disc at the level of entry | Sinuvertebral nerves, formed by a somatic root from ventral ramus and an autonomic root from grey ramus communicans. An ascending branch passes as far as the above vertebral disc. A descending branch supplies the disc at the level of entry | ||
==Fusion== | ==Fusion Surgery== | ||
There are no sham controlled studies whatsoever for fusion surgery. There are not even any randomised controlled trials with an active control when disc pain has been proven. RCTs on non specific low back pain with an active control were negative.<ref>Harris IA, Traeger A, Stanford R, Maher CG, Buchbinder R. Lumbar spine fusion: what is the evidence?. Intern Med J. 2018;48(12):1430-1434. doi:10.1111/imj.14120</ref> Therefore the benefit of fusion surgery for proven disc pain is unknown, and such surgery has no basis in any high level evidence. | There are no sham controlled studies whatsoever for fusion surgery. There are not even any randomised controlled trials with an active control when disc pain has been proven. RCTs on non specific low back pain with an active control were negative.<ref>Harris IA, Traeger A, Stanford R, Maher CG, Buchbinder R. Lumbar spine fusion: what is the evidence?. Intern Med J. 2018;48(12):1430-1434. doi:10.1111/imj.14120</ref> Therefore the benefit of fusion surgery for proven disc pain is unknown, and such surgery has no basis in any high level evidence. | ||
Revision as of 09:41, 12 July 2020
A variety of radiofrequency procedures have been developed for the treatment of discogenic pain. An ongoing limitation is the lack of a gold standard for proving discogenic pain, and the term "precision treatment" refers to treatment of a proven pain generator unlike treating "non-specific low back pain." Provocation discography is generally used in research but this procedure has its issues. Leggett et al in 2015 found mixed evidence for radiofrequency procedures for discogenic pain.[1] Helm et al in 2019 concluded that there was level 1 evidence for the use of biacuplasty, and level 3 evidence for intradiscal electrothermal annuloplasty for the treatment of discogenic pain.[2] The author is not aware of any Musculoskeletal Medicine specialists in New Zealand using radiofrequency procedures for discogenic pain.
Lumbar Disc Innervation
Sinuvertebral nerves, formed by a somatic root from ventral ramus and an autonomic root from grey ramus communicans. An ascending branch passes as far as the above vertebral disc. A descending branch supplies the disc at the level of entry
Fusion Surgery
There are no sham controlled studies whatsoever for fusion surgery. There are not even any randomised controlled trials with an active control when disc pain has been proven. RCTs on non specific low back pain with an active control were negative.[3] Therefore the benefit of fusion surgery for proven disc pain is unknown, and such surgery has no basis in any high level evidence.
Radiofrequency Procedures
Cooled Radiofrequency Biacuplasty
Two cooled RF electrodes are placed on the posterolateral sides of the annulus to coagulate the nociceptors of the neo-innervated tissue. A dumbbell shape is formed between the two RF probes to cover the posterior annulus. This procedure produces internal disc temperatures in excess of 45° C. Kapural et al used a setting of 50° C for 15 minutes, followed by individual monopolar lesions (RF energy transferred via one probe at a time in sequence) to extend the lateral extent of the central lesion set at 60°C for 2.5 minutes. They used intravenous sedation including midazolam, fentanyl, or propofol. But during the active heating portion of biacuplasty, subjects were awake and indicated whether pain was localized to the lesion area or if they had any other symptoms.[4]
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Kapural et al 2013[4] |
59 |
|
Positive provocative discography and negative control. |
✅Positive study 6 months: Mean NRS decrease 2.78 vs 1.32, mean SF-36 increase 15. no significant improvement in ODI (except in post hoc <40 yo patients) Success: 29.6% vs 3.3% (15 point increase in SF-36 and 2 reduction in NRS |
|
| Desai et al 2016[5] |
63 |
|
Provocation discography |
✅Positive study 6 months: Mean NRS decrease -2.4 vs -0.56, Treatment response 50% vs 18% 12 months: Mean NRS decrease -2.2, Treatment response 50% SF36 + 64% ODI |
|
Intradiscal Electrothermal Annuloplasty
in IDET a resistive coil is placed between the annulus and nucleus and along the posterior annulus. It is heated to 90 degrees, Putatively seals the fissure and denatures the annulus.
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Freeman 2005[6] |
57 |
|
Provocation CT discography with discrete annular tear or global degeneration |
❌Negative study up to 6 months |
|
| Pauza 2004[7] |
64 |
|
CT Provocation discography with posterior annular tear only |
❓ “Positive” study, but modest improvements only
|
|
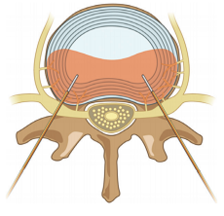
Lumbar Disc IN, discTRODE, Ramus Communicans RF
- DiscTRODE™ (radio-frequency electrode) is positioned within the posterior annulus
- The RF electrode is positioned in the middle of the nucleus. Temperature achieved may not be sufficient to denervate posterior annulus when the heat source is inside the nucleus
| Study | N | Arms | Selection Criteria | Results |
|---|---|---|---|---|
| Barendse et al, 2001 (RCT)[8] |
13 |
|
1 x positive analgesic discography (>50% relief) |
❌Negative study at 2 months |
| Kvarstein et al, 2009 (RCT)[9] |
10 |
|
1 x positive concordant provocation discography (pain >7/10 at 1/3 levels) |
❌ Negative study up to 12 months |
| Van Tilburg 2017, (RCT)[10] |
60 |
|
1 x positive block at ramus communicans (decrease NRS 2 or more, placement confirmed with sensory and motor stimulation) |
❌Negative study at 3 months |
Also Ercelen evaluted 120 vs 360 seconds at 80 degrees and found no difference.[11]
Mixed Radiofrequency Studies
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Juch et al 2017[12] |
202 |
|
Positive provocative discography and negative control. |
❌Negative study |
|
Bottom Line
- Biacuplasty [Level 1]
- IDET [Level 3]
- intradiscal RF[Level 5]
- discTRODE [Level 5]
- Ramus communicans RF [Level 5]
- Fusion Surgery [Level 5]
Quiz
See Also
- Sacroiliac Joint Precision Treatment
- Lumbar Facet Joint Precision Treatment
- Radiofrequency Neurotomy
References
- ↑ Leggett LE, Soril LJ, Lorenzetti DL, et al. Radiofrequency ablation for chronic low back pain: a systematic review of randomized controlled trials. Pain Res Manag. 2014;19(5):e146-e153. doi:10.1155/2014/834369
- ↑ Helm Ii S, Simopoulos TT, Stojanovic M, Abdi S, El Terany MA. Effectiveness of Thermal Annular Procedures in Treating Discogenic Low Back Pain. Pain Physician. 2017;20(6):447-470…. and my opinion for Ramus communicans RF.
- ↑ Harris IA, Traeger A, Stanford R, Maher CG, Buchbinder R. Lumbar spine fusion: what is the evidence?. Intern Med J. 2018;48(12):1430-1434. doi:10.1111/imj.14120
- ↑ 4.0 4.1 Kapural L, Vrooman B, Sarwar S, et al. A randomized, placebo-controlled trial of transdiscal radiofrequency, biacuplasty for treatment of discogenic lower back pain. Pain Med. 2013;14(3):362-373. doi:10.1111/pme.12023
- ↑ Desai MJ, Kapural L, Petersohn JD, et al. A Prospective, Randomized, Multicenter, Open-label Clinical Trial Comparing Intradiscal Biacuplasty to Conventional Medical Management for Discogenic Lumbar Back Pain. Spine (Phila Pa 1976). 2016;41(13):1065-1074. doi:10.1097/BRS.0000000000001412
- ↑ Freeman BJ. IDET: a critical appraisal of the evidence. Eur Spine J. 2006;15 Suppl 3(Suppl 3):S448-S457. doi:10.1007/s00586-006-0156-2
- ↑ Pauza KJ, Howell S, Dreyfuss P, Peloza JH, Dawson K, Bogduk N. A randomized, placebo-controlled trial of intradiscal electrothermal therapy for the treatment of discogenic low back pain. Spine J. 2004;4(1):27-35. doi:10.1016/j.spinee.2003.07.001
- ↑ Barendse GA, van Den Berg SG, Kessels AH, et al. Randomized controlled trial of percutaneous intradiscal radiofrequency thermocoagulation for chronic discogenic back pain: Lack of effect from a 90-second 70 C lesion. Spine 2001;26:287-92.
- ↑ Kvarstein G, Mawe L, Indahl A, et al. A randomized double-blind controlled trial of intra-annular radiofrequency thermal disc therapy – a 12-month follow-up. Pain 2009;145:279-86
- ↑ van Tilburg CW, Stronks DL, Groeneweg JG, Huygen FJ. Randomized sham-controlled, double-blind, multicenter clinical trial on the effect of percutaneous radiofrequency at the ramus communicans for lumbar disc pain. Eur J Pain. 2017;21(3):520-529. doi:10.1002/ejp.945
- ↑ Erçelen O, Bulutçu E, Oktenoglu T, et al. Radiofrequency lesioning using two different time modalities for the treatment of lumbar discogenic pain: a randomized trial. Spine (Phila Pa 1976). 2003;28(17):1922-1927. doi:10.1097/01.BRS.0000083326.39944.73
- ↑ Juch JNS, Maas ET, Ostelo RWJG, et al. Effect of Radiofrequency Denervation on Pain Intensity Among Patients With Chronic Low Back Pain: The Mint Randomized Clinical Trials [published correction appears in JAMA. 2017 Sep 26;318(12 ):1188]. JAMA. 2017;318(1):68-81. doi:10.1001/jama.2017.7918