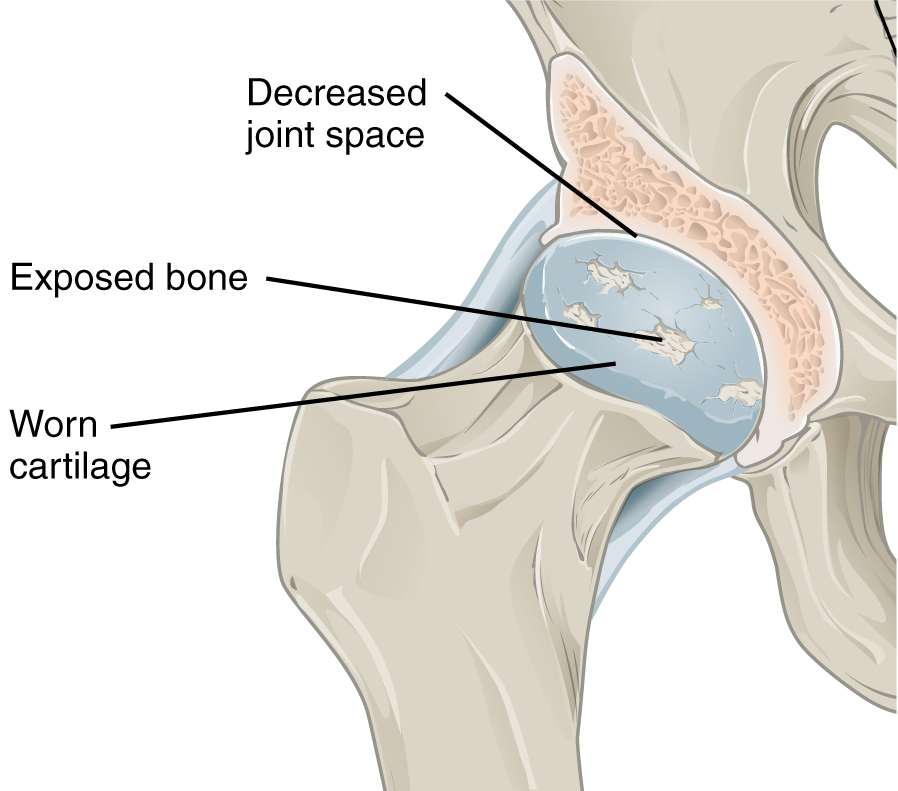
Hip Osteoarthritis
| |
| Hip Osteoarthritis | |
|---|---|
| Epidemiology | ~4% symptomatic OA, ~20% radiographic OA, in age >50. |
| Tests | Diagnostic intra-articular hip joint local anaesthetic injection |
Epidemiology
A US study of mostly Caucasian people aged over 50, the prevalence of radiographic hip OA was 19.6%, and the prevalence of symptomatic disease was 4.2%, with the prevalence increasing with higher age. The authors found a male predominance of symptomatic OA, especially in older individuals, unlike other studies which have tended to find a female predominance. There is generally a male predominance of radiographic OA.[1] A Japanese study found the prevalence of radiographic hip osteoarthritis to be 18.2% in men and 14.3% in women[2]
Aetiopathogenesis
There are several structures around the hip that are richly innervated by sensory nerve fibres. These include the periosteum, subchondral bone, synovium, and surrounding soft tissues. In the presence of Central Sensitisation there may be an additional central physiological process. Hip osteoarthritis can also lead to changes in gait which can lead to pain in the knees and lumbar spine.[3]
Higher bone density can drive knee osteoarthritis but not hip osteoarthritis
Clinical Features
History
The pain is often poorly localised. Patients can have pain over quite a large area including the front of the thighs, groin, lateral thighs, buttocks, and the posterior upper thighs. Patients with Central Sensitisation can have unusual distributions of pain at a surprising distance from the hip such as below the knee.
There is no clear association between pain levels and radiographic severity of hip osteoarthritis. Up to 40% of patients with hip osteoarthritis have no pain. Patients with higher pain levels showed differences in sensitisation as measured by quantitative sensory testing.[4]
None of the features on history are particularly helpful on their own for identifying hip OA. Medial thigh pain is highly suggestive of hip OA but is only present in 2.7% of patients. The presence of morning stiffness, pain on walking, and relief of pain on sitting all have positive likelihood ratios of <2.0, but their negative likelihood ratios are more helpful, i.e. the absence of these factors.[3]
| Feature on History | Sensitivity | Specificity | LR+ | LR- |
|---|---|---|---|---|
| Family history of OA | 34% | 84% | 2.1 [95% CI, 1.2-3.6] |
0.79 [95% CI, 0.67-0.93] |
| Personal history of knee OA | 33% | 84% | 2.1 [95%CI, 1.1-3.8] |
0.80 [95% CI, 0.68-0.95] |
| Age > 60 | 96% | 25% | 1.5 [95% CI, 1.3-1.7] |
0.11 [95% CI, 0.02-0.78] |
| Age < 50 | 91% | 28% | 1.3 [95% CI, 1.1-1.5] |
0.32 [95% CI, 0.16-0.62] |
| Worst pain in medial thigh | 12% | 98% | 7.8 [95%CI, 1.7-37] |
0.89 [95%CI, 0.77-1.0] |
| Worst pain in buttock | 12-67% | 57-69% | 0.38-2.0 | 0.38-0.76 |
| Pain on climbing stairs or walking down slopes | 68% | 68% | 2.1 [95%CI, 1.6-2.8] |
0.47 [95%CI, 0.35-0.63] |
| Morning stiffness <60 min | 56-91% | 41-67% | 1.5-1.7 | 0.22-0.65 |
| Pain on initial steps after rest | 92% | 26% | 1.2 [95%CI, 1.1-1.4] |
0.31 [95%CI, 0.08-1.2] |
| Pain on walking | 80-97% | 12-34% | 1.1-1.2 | 0.25-0.58 |
| Pain relieved by sitting | 92% | 33% | 1.4 [95%CI, 0.2-1.6] |
0.24 [95%CI, 0.06-0.92] |
Examination
- Main article: Hip Examination
Physical examination findings are in general more useful than historical features for identifying hip OA. Posterior hip pain is the test with the highest likelihood ratio, but some patients may not be very excited about trying this. Groin pain on hip abduction or adduction, abductor weakness, decreased hip adduction, and decreased hip internal rotation are all findings with positive likelihood ratios above 3. For identifying those who do not have hip OA, normal hip passive adduction or abduction are the most helpful.[3]
Extension is examined with the patient prone and lifting the leg off the table. Flexion is examined with the patient supine, and the examiner lifts the knee to the abdomen. In this position the foot can be kept in the same position, and the knee moved towards the midline, causing internal rotation. The hip can then be moved away from the midline, which causes external rotation. Adduction and abduction are assessed by putting the feet together. The foot is then moved across or away from the midline respectively. Normal ranges of motion are below. Goniometers are sometimes used, but usually estimates are sufficient. The examiner should compare range to the other side, but keeping in mind that osteoarthritis is often bilateral.[3]
| Passive Movement | Normal ROM |
|---|---|
| Flexion | 0 - 140° |
| Internal rotation | 0 - 30° |
| External rotation | 0 - 40° |
| Abduction | 0 - 50° |
| Adduction | 0 - 30° |
| Extension | 0 - 20° |
| Feature on Exam | Sensitivity | Specificity | LR+ | LR- |
|---|---|---|---|---|
| Abductor weakness | 44 | 90 | 4.5 | 0.62 |
| Limp | 85 | 43 | 1.5 | 0.35 |
| Inguinal ligament tenderness | 60 | 75 | 2.4 | 0.53 |
| Tensor fascia lata tenderness | 40 | 80 | 2.0 | 0.75 |
| Squat causing posterior pain | 24 | 96 | 6.1 | 0.79 |
| Groin pain on abduction or adduction | 33 | 94 | 5.7 | 0.71 |
| Scour test | 62 | 74 | 2.4 | 0.51 |
| Pain on hip adduction | 68-80 | 46-54 | 1.5 | 0.43-0.59 |
| Pain on hip internal rotation | 82-88 | 38-39 | 1.4 | 0.31-0.45 |
| Restricted movement in 3 planes | NA | NA | 4.4 | NA |
| Restricted movement in 2 planes | NA | NA | 1.5 | NA |
| Restricted movement in 1 plane | NA | NA | 1.3 | NA |
| Restricted movement in 0 planes | NA | NA | 0.91 | NA |
| Decreased hip adduction | 80 | 81 | 4.2 | 0.25 |
| Decreased hip internal rotation | 66 | 79 | 3.2 | 0.43 |
| Decreased hip range of movement | 75 | 74 | 2.9 | 0.34 |
| Decreased hip extension | 76 | 68 | 2.4 | 0.35 |
| Decreased hip external rotation | 76 | 64 | 2.1 | 0.37 |
| Decreased hip abduction | 88 | 46 | 1.6 | 0.26 |
Combinations of findings have also been studied.
| Findings | +LR | -LR |
|---|---|---|
|
35 (5 or more findings) | 0.05 (3 or fewer findings) |
|
4.9 (4 or more findings) | 0.24 (0 or 1 findings) |
Imaging
Plain radiographs can demonstrate joint space narrowing, osteophytes, subchondral sclerosis, and subchondral cysts. They may also show alternative causes for pain such as pelvic bone tumours. Plain radiographs are cheap, however because most patients with radiographic OA have asymptomatic disease, there is a risk of incorrectly attributing the pain to osteoarthritis, and subsequently having incorrect treatment. Therefore it is as important as ever to consider the pre-test probability, and consider other diagnoses.
Laboratory Tests
Depending on the clinical context, rheumatological blood tests may need to be performed.
Diagnosis
The diagnosis can be made clinically in those with mild to moderate symptoms. In those with more severe symptoms then plain radiographs are performed. If the radiographs are normal then there should be a search for other causes of pain.
A commonly performed procedure in Musculoskeletal Medicine in New Zealand is the diagnostic intra-articular hip joint injection. Under either ultrasound or fluoroscopic guidance, local anaesthetic is infiltrated into the hip joint. An appreciable reduction in pain post-procedure is consistent with nociception arising from the hip joint.
Differential Diagnosis
- Anterior pain
- Hip Osteoarthritis
- Femoroacetabular Impingement
- Iliopsoas Tendionopathy
- Inflammatory arthritis
- Avascular necrosis/osteonecrosis of the femoral head
- Hip Labral Tear
- Nerve Entrapments: Genitofemoral Nerve Entrapment, Ilioinguinal Nerve Entrapment
- Developmental Dysplasia of the Hip
- Transient Osteoporosis of the Hip
- Inguinal or femoral hernia
- Gynaecological causes
- Gonadal tumours
- Inguinal lymphadenopathy
- Posterior pain
- Lateral pain
- Medial pain
- Other
- Septic Arthritis
- Hip Fracture
- Hip chondral defects
- Ligamentum teres injury
- Pelvic bone tumours
- Pelvic insufficiency fractures
- Stress fracture
- Peripheral Vascular Disease
- Fibromyalgia
- Leaking abdominal aortic aneurysm
Prognosis
- A minority have clear cut clinical and radiological recovery, especially with marked osteophytosis and concentric disease
- Superolateral migration of the femoral head is correlated with more rapid osteoarthritis progression, also with atrophic bone response
Treatment
Total hip joint replacement is usually effective for reducing pain. However 10% of patients have chronic postsurgical pain, and preoperative central sensitisation has been thought to be a risk factor for this.[4]
Resources
- Dieppe PA good author to read
- Media:Hip_Osteoarthritis_-_JAMA_Rational_Clinical_Examination_2019.pdf
References
- ↑ Kim et al.. Prevalence of radiographic and symptomatic hip osteoarthritis in an urban United States community: the Framingham osteoarthritis study. Arthritis & rheumatology (Hoboken, N.J.) 2014. 66:3013-7. PMID: 25103598. DOI. Full Text.
- ↑ Iidaka et al.. Prevalence of radiographic hip osteoarthritis and its association with hip pain in Japanese men and women: the ROAD study. Osteoarthritis and cartilage 2016. 24:117-23. PMID: 26241774. DOI.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Metcalfe et al.. Does This Patient Have Hip Osteoarthritis?: The Rational Clinical Examination Systematic Review. JAMA 2019. 322:2323-2333. PMID: 31846019. DOI. Full Text.
- ↑ 4.0 4.1 Hattori T, Shimo K, Niwa Y, Tokiwa Y, Matsubara T. Association of Chronic Pain with Radiologic Severity and Central Sensitization in Hip Osteoarthritis Patients. J Pain Res. 2021;14:1153-1160 DOI
Literature Review
- Reviews from the last 7 years: review articles, free review articles, systematic reviews, meta-analyses, NCBI Bookshelf
- Articles from all years: PubMed search, Google Scholar search.
- TRIP Database: clinical publications about evidence-based medicine.
- Other Wikis: Radiopaedia, Wikipedia Search, Wikipedia I Feel Lucky, Orthobullets,


