Lumbar Zygapophysial Joint Precision Treatment
Introduction
This article deals with the treatment of lumbar facet joint pain when diagnosed by a precision diagnosis technique. CT or fluoroscopic guidance is mandatory.
Facet Joint Innervation
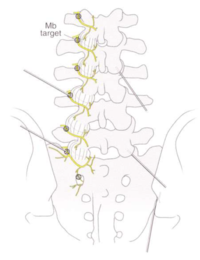
Because each facet joint receives dual innervation from two different medial branches, in order to eliminate all sensory supply to a particular facet joint, you need to perform radiofrequency ablation (neurotomy) on two separate medial branches. Each facet joint is supplied by a descending medial branch and an ascending medial branch. However the L5 dorsal ramus has no medial branch, and so blocks and radiofrequency techniques are applied to the dorsal ramus itself.
For example, the L4/5 segment
- Foramen: exiting L4 nerve
- L4 dorsal ramus medial branch innervates the L4/5 facet joint and the below L5/S1 facet joint.
- The below L5/S1 facet also receives innervation from the L5 dorsal ramus
In other words, each medial branch innervates same level and below. And so you block the same level and above.
Intraarticular Injections
There is only one negative RCT for the treatment of lumbar facet joint pain when the diagnosis was made by a precision diagnosis technique.
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Carette et al 1991 (RCT)[1] | 97 |
|
1 x positive intraarticular block (>50% pain relief) | ❌Negative study
No statistical difference in pain or function. (42% vs 33%) Only 22% vs 10% sustained improvement from month 1 to 6 in responders. |
|
Therapeutic Medial Branch Blocks
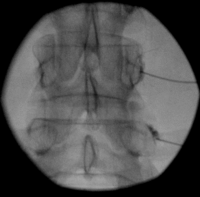
Medial branch block at the right L4/L5 level.
Medial branch blocks can have a therapeutic effect on their own without progressing to radiofrequency neurotomy. The exact mechanism of this is unknown.
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Manchikanti 2008 + 2010(RCT)[2] | 120 |
|
2 x comparative blocks (>80% pain relief) | ✅Both improved.
At 2 years 85% vs 90% improvement in NRS, and 87% vs 88% improvement in ODI. Average relief 19 weeks, average number of procedures 5-6 |
|
| Manchikanti 2001 (RCT)[3] | 73 |
|
2 x comparative blocks | ✅Both improved. average 6 procedures over 12 months. Range of pain relief 2 to 102 weeks. |
|
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Cohen 2018, (RCT) [4] | 229 |
|
IAB + MBB: (>50% relief)
and negative outcome progressed to RF, plus all saline group. |
❌single injection not effective long term |
|
Radiofrequency Neurotomy Procedures
Radiofrequency neurotomy for lumbar facet joint pain is controversial in some circles. Systematic reviews differ in their conclusions. Cochrane in 2015 found modest benefit but they did not differentiate between studies with different selection techniques. Studies selecting by a single positive medial branch block with have large numbers of false positives, and this was not evaluated in the Cochrane analysis.[5]Manchikanti et al designated the procedure at level 2 evidence,[6] while Scheider et al concluded that there is a difference in outcome depending on patient selection criteria[7] In general, selection should be based on at least 80% relief from two medial branch blocks.[7] It is highly operator and technique dependent and results can depend on the use of a larger 16G probe, making multiple lesions, and using a parallel technique.
Selection by One Positive Intraarticular Block
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Leclair 2001 (RCT)[8] | 70 |
|
1 x IAB with steroid (“significant relief”) | ❌Negative study |
|
| Van Wijk 2005, (RCT)[9] |
81 |
|
1 x IAB (>50% relief) |
❌Negative study |
|
|
Cohen 2018, (RCT) [4] |
229 |
|
IAB + MBB: (>50% relief), and negative outcome progressed to RF, plus all saline group. |
✅ IAB + MBB > Saline for predicting RF success 3 months: success 51%, 56%, 24% 6 months: success 31%, 42%, 17% |
|
|
Gallagher 1994, (RCT)[10] |
41 |
|
?IAB (article not accessible) |
✅ Positive study |
|
|
Lakemeier 2013, (RCT)[11] |
56 |
|
IAB (>50% relief) |
❌Negative study |
|
Selection by One Positive Medial Branch Block
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Van Kleef 1999, (RCT)[12] | 31 |
|
1 x MBB (>50% relief) | ✅Positive study. Success 66.7% vs 37.5% at 8 weeks. Mean -1.94 difference
But independent analysis showed statistically insignificant due to small sample size. |
Incorrect technique (orthogonal rather than parallel probe) |
| Van Tilburg 2016, (RCT) [13] |
60 |
|
1 x MBB (≥2 reduction in NRS) |
❌ Difference at 1 month but not 3 months |
|
|
Cohen 2018, (RCT)[4] |
229 |
|
IAB + MBB: (>50% relief), with positive block but negative outcome progressed to RF, plus all saline group. |
✅ IAB + MBB > Saline for predicting RF success 3 months: success 51%, 56%, 24% 6 months: success 31%, 42%, 17% |
|
|
Juch 2017, (RCT)[14] |
251 |
|
1 x MBB (>50% relief) |
Equal outcomes |
|
|
Tekin 2007, (RCT)[15] |
60 |
|
1 x MBB (>50% relief) |
|
No categorical data on success rates using a validated objective quantitative measure, it was excluded from the final analysis |
|
McCormick 2019, (RCT)[16] |
43 |
|
1 x MBB (>75% relief) |
Equal outcomes (52% vs 47% at 6 months with >50% NRS reduction) |
|
Selection by Two Positive Medial Branch Block
| Study | N | Arms | Selection Criteria | Results | Comments |
|---|---|---|---|---|---|
| Cohen 2010, (RCT) [17] | 151 |
|
>50% relief | ✅>50% relief of pain in 33% (0 blocks), 39% (1 block), and 64% (dual) at 3 months |
|
| Nath 2008, (RCT) [18] | 40 |
|
two positive MBBs (>80% relief) | ✅Mean pain relief 1.9 compared to 0.4. |
|
| Moussa 2016, (RCT). [19] | 120 |
|
2 x positive blocks (Near or near complete relief) | ✅ 1 year: Success (Common outcome) 67.5% vs 57.5% vs 10%
3 years: 57.5% vs 17.5% vs 2.5% (capsule RF superior) |
|
There are variable quality non-RCT studies suggesting that the greatest chance of success is when selection is based on two positive medial branch blocks.[7] Of particular note to New Zealand, MacVicar published results that when selection was based on dual blocks of 100% pain relief, there was a 56% chance of 100% pain relief, back to work, and no further spinal care.[20]
Bottom Line
- Intraarticular injections [Level 4]
- Therapeutic blocks +/- repeated [Level 2]
- Lumbar RF ablation [Level 2], but patients must be selected by two positive medial branch blocks with >80% pain relief
Quiz
See Also
References
- ↑ Carette S, Marcoux S, Truchon R, et al. A controlled trial of corticosteroid injections into facet joints for chronic low back pain. N Engl J Med. 1991;325(14):1002-1007. doi:10.1056/NEJM199110033251405
- ↑ Manchikanti L, Singh V, Falco FJ, Cash KA, Fellows B. Comparative outcomes of a 2-year follow-up of cervical medial branch blocks in management of chronic neck pain: a randomized, double-blind controlled trial. Pain Physician. 2010;13(5):437-450.
- ↑ Manchikanti L, Pampati V, Bakhit CE, et al. Effectiveness of lumbar facet joint nerve blocks in chronic low back pain: a randomized clinical trial. Pain Physician. 2001;4(1):101-117.
- ↑ 4.0 4.1 4.2 Cohen SP, Doshi TL, Constantinescu OC, et al. Effectiveness of Lumbar Facet Joint Blocks and Predictive Value before Radiofrequency Denervation: The Facet Treatment Study (FACTS), a Randomized, Controlled Clinical Trial [published correction appears in Anesthesiology. 2018 Sep;129(3):618]. Anesthesiology. 2018;129(3):517-535. doi:10.1097/ALN.0000000000002274
- ↑ Maas ET, Ostelo RW, Niemisto L, et al. Radiofrequency denervation for chronic low back pain. Cochrane Database Syst Rev. 2015;(10):CD008572. Published 2015 Oct 23. doi:10.1002/14651858.CD008572.pub2
- ↑ Manchikanti L, Kaye AD, Soin A, et al. Comprehensive Evidence-Based Guidelines for Facet Joint Interventions in the Management of Chronic Spinal Pain: American Society of Interventional Pain Physicians (ASIPP) Guidelines Facet Joint Interventions 2020 Guidelines. Pain Physician. 2020;23(3S):S1-S127.
- ↑ 7.0 7.1 7.2 7.3 Schneider BJ, Doan L, Maes MK, Martinez KR, Gonzalez Cota A, Bogduk N. Systematic review of the effectiveness of lumbar medial branch thermal radiofrequency neurotomy, stratified for diagnostic methods and procedural technique. Pain Med 2020 Feb 10. [Epub ahead of print]
- ↑ Leclaire R, Fortin L, Lambert R, et al. Radiofrequency facet joint denervation in the treatment of low back pain: a placebo-controlled clinical trial to assess efficacy. Spine 2001;26(13):1411-6
- ↑ van Wijk RMA, Geurts JWM, Wynne HJ, et al. Radiofrequency denervation of lumbar facet joints in the treatment of chronic low back pain. A randomized, double-blind sham lesion-controlled trial. Clin J Pain 2005;21(4):335-4
- ↑ Gallagher J, Petriccione di Vadi PL, Wedley JR. Radiofrequencyfacet joint denervation in the treatment of low back pain: aprospective controlled double-blind study to assess its efficacy.The Pain Clinic 1994;7:193-8.
- ↑ Lakemeier S, Lind M, Schultz W, Fuchs-Winkelmann S,Timmesfeld N, Foelsch C, et al. A comparison of intraarticularlumbar facet joint steroid injections and lumbar facet jointradiofrequency denervation in the treatment of low back pain:a randomized, controlled, double-blind trial. Anesthesia &Analgesia 2013;117(1):228-35.
- ↑ van Kleef M, Barendse GA, Kessels A, Voets HM, Weber WE, de Lange S. Randomized trial of radiofrequency lumbar facet denervation for chronic low back pain. Spine (Phila Pa 1976). 1999;24(18):1937-1942. doi:10.1097/00007632-199909150-00013
- ↑ van Tilburg CW, Stronks DL, Groeneweg JG, Huygen FJ. Randomised sham-controlled double-blind multicentre clinical trial to ascertain the effect of percutaneous radiofrequency treatment for lumbar facet joint pain. Bone Joint J. 2016;98-B(11):1526-1533. doi:10.1302/0301-620X.98B11.BJJ-2016-0379.R2
- ↑ Juch JNS, Maas ET, Ostelo RWJG, et al. Effect of Radiofrequency Denervation on Pain Intensity Among Patients With Chronic Low Back Pain: The Mint Randomized Clinical Trials [published correction appears in JAMA. 2017 Sep 26;318(12 ):1188]. JAMA. 2017;318(1):68-81. doi:10.1001/jama.2017.7918
- ↑ Tekin I, Mirzai H, Ok G, Erbuyun K, Vatansever D. A comparison of conventional and pulsed radiofrequency denervation in the treatment of chronic facet joint pain. Clin J Pain 2007;23:524–9.
- ↑ McCormick ZL, Choi H, Reddy R, et al. Randomized prospective trial of cooled versus traditional radiofrequency ablation of the medial branch nerves for the treatment of lumbar facet joint pain. Reg Anesth Pain Med. 2019;44(3):389-397. doi:10.1136/rapm-2018-000035
- ↑ Cohen SP, Williams KA, Kurihara C, et al. Multicenter, randomized, comparative cost-effectiveness study comparing 0, 1, and 2 diagnostic medial branch (facet joint nerve) block treatment paradigms before lumbar facet radiofrequency denervation. Anesthesiology 2010;113(2):395–405
- ↑ Nath S, Nath CA, Pettersson K. Percutaneous lumbar zygapophysial (facet) joint neurotomy using radiofrequency current, in the management of chronic low back pain. A randomized double-blind trial. Spine 2008;33:1291–7 But did not report any data from which success rates could be calculated. Positive study. Mean pain relief 1.9 compared to 0.4.
- ↑ Moussa WM, Khedr W. Percutaneous radiofrequency facet capsule denervation as an alternative target in lumbar facet syndrome. Clin Neurol Neurosurg. 2016;150:96-104. doi:10.1016/j.clineuro.2016.09.004
- ↑ MacVicar J, Borowczyk JM, MacVicar AM, Loughnan BM, Bogduk N. Lumbar medial branch radiofrequency neurotomy in New Zealand. Pain Med. 2013;14(5):639-645. doi:10.1111/pme.12000