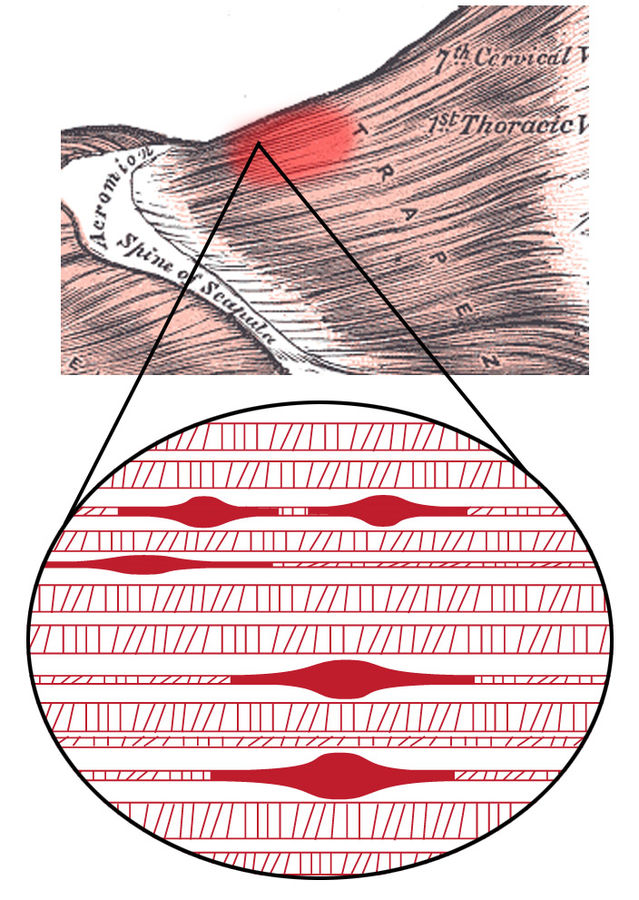
Myofascial Pain Syndrome
Myofascial pain syndrome is pain that arises from muscles or related fascia and is characterised by the presence of myofascial trigger points (MTPs).
Definition
Myofascial Pain: is pain that arises from muscles or related fascia.
Myofascial trigger point: A palpable hypersensitive tender nodule in a taut skeletal muscle band with a twitch response. Pressure can also cause a characterised referred pain pattern, motor dysfunction, and autonomic responses (e.g. vasodilation, vasoconstriction, piloerection).
A MTP can be latent or active.
- Active MTPs: Spontaneously painful with increased pain on contraction or stretching of the muscle
- Latent MTPs: Focal tender and tight areas that aren't spontaneously painful but may restrict range of motion and strength
Pathophysiology
The pathophysiology isn't completely known and is controversial. The MTP is associated with endplate noise from a motor endplate that releases abnormal amounts of acetylcholine. Sarcomeres are shortened in the endplate regions which cause a local release of sensitising substances resulting in pain.
They are often related to nociplastic pain and allodynia/hyperalgesia.
Clinical Assessment
Clinical Features
Palpation: The MTP should be palpated perpendicular to the direction of the muscle fibre. When palpating over a firm or bony structure compress the muscle against it. In some areas the muscle can be grasped between the fingers with a pincer grip to allow for MTP palpation. Referred pain is most readily detected with palpation in the centre of the MTP. So move your fingers along the taut band to find the hardest and most tender spot.
Referred Pain: When found compress it for 5-10 seconds and ask the patient if there is local or referred pain. Referred pain is somewhat follows the myotome pattern of innervation. For example, infraspinatus is primarily innervated by C5, and tends to refer pain to other C5-innervated muscles, with also a spread to C4 and C6 muscles (Also see Deep Somatic Pain).
Twitch Response: A local twitch response can occur which is when pressure over the MTP causes localised contraction. It is a brief (25-250ms), high-amplitude, polyphasic electrical discharge. It is dependent on an intact spinal cord reflex arc. It isn't seen in healthy muscle.[1]
Weakness and ROM Restriction: There may be increased tension and shortening with restricted range of motion and weakness with poor muscle activation patterns. MTPs typically occur in muscles that are fatigued, overloaded, weak, or activated because of failure of other muscles. Weakness can be temporarily reversed with inactivation of the trigger point.
Autonomic Changes: There can be vasodilation or vasoconstriction due to autonomic nervous system activation. This can be seen as erythema or blanching.
Clinical Syndromes
In a myofascial pain syndrome there may be just one trigger point but more typically there are several trigger points.
Low back Pain:
- Quadratus lumborum: low back with radiation into the legs or testicles
- Iliopsoas: vertical band in low back and upper anterior thigh
- Gluteus medius: sacral and buttock area and lateral hip
Neck and Shoulder Pain:
- Trapezius: upper trapezius refers pain to the back of the neck and angle of the jaw
- Levator scapula: angle of the neck and shoulder
Hip Pain:
- Gluteus medius
- Gluteus minimus
Pelvic Pain:
- Levator ani
Headaches
- Sternocleidomastoid: anterior face and supraorbital area
- Upper trapezius: vertex of the forehead and temple
- Deep cervical muscles: post-occipital and retro-orbital pain
Jaw Pain:
- Masseters and Pterygoids
- Upper trapezius and sternocleidomastoid
Upper Limb Pain:
- Subscapularis
- Infraspinatus
- Teres Major
- Serratuis Anterior
- Pectoralis minor: radiating pain down the ulnar side of the arm into the little finger.
Lower Limb Pain:
- Tensor fascia lata: lateral thigh pain
- Iliotibial band: lateral knee pain
- Quradriceps: anterior knee pain
- Hamstring and popliteus: posterior knee pain
- Anterior tibialis: anterior leg pain
- Peroneus longus: lateral ankle pain
Chest and Abdominal Pain:
NB: MTPs can accompany true visceral pathology (see Visceral Pain)
- Pectoralis major: ipsilateral anterior chest pain with radiation down the ulnar side of the arm
- Sternalis: deep substernal pain
- Rectus abdominis: abdominal pain
Investigations
Blood tests can include TSH, ferritin, vitamin D, and vitamin B12.
Diagnosis
The first three are essential for the diagnosis, the last five are not required.[1]
- Taut band within the muscle
- Exquisite tenderness at a point on the taut band
- Reproduction of the patient’s pain
- Local twitch response
- Referred pain
- Weakness
- Restricted range of motion
- Autonomic signs: skin warmth or erythema, tearing, piloerection.
A pragmatic definition is the presence of a tender taut band that reproduces the patient's pain in full or in part.
Treatment
Posture and Ergonomics
Correct any predisposing factors.
Manual Therapy
Manual therapy can be used to improve range of motion, but this may not necessarily improve pain.[2]
- Muscle energy techniques including Postisometric relaxation
- Ischaemic compression
- Stretching
- Strain-counterstrain technique
- Positional release technique
- Pressure release
- Transverse friction massage
- Joint manipulation
Treatment of an MTP depends on the cause
- Muscle is weak and fatigues quickly: treatment is strengthening
- Muscle is overactive and compensating for other muscles that aren't correctly activating: restore correct motor pattern for example scapula stabilisation
- Muscle is inappropriately active: modify inappropriate activities that are overloading the muscle e.g. holding one's phone between the head and shoulder.
Trigger Point Injection
The trigger point is peppered with lidocaine![]() using a fine needle to inactivate the trigger point. The MTP is accurately located by finding a local twitch response with the needle tip.
using a fine needle to inactivate the trigger point. The MTP is accurately located by finding a local twitch response with the needle tip.
Medications
Options are NSAIDs and tricyclic antidepressants.
See Also
- triggerpoints.net
- Central Sensitisation
- Allodynia and hyperalgesia
- Fibromyalgia
- Deep Somatic Pain
- Critical Overview MPS 2019
- Critical overview MPS - dommerholt 2017
References
- ↑ 1.0 1.1 Gerwin RD. Diagnosis of myofascial pain syndrome. Phys Med Rehabil Clin N Am. 2014 May;25(2):341-55. doi: 10.1016/j.pmr.2014.01.011. Epub 2014 Mar 18. PMID: 24787337.
- ↑ Guzmán-Pavón MJ, Cavero-Redondo I, Martínez-Vizcaíno V, Torres-Costoso AI, Reina-Gutiérrez S, Álvarez-Bueno C. Effect of Manual Therapy Interventions on Range of Motion Among Individuals with Myofascial Trigger Points: A Systematic Review and Meta-Analysis. Pain Med. 2022 Jan 3;23(1):137-143. doi: 10.1093/pm/pnab224. PMID: 34289061.