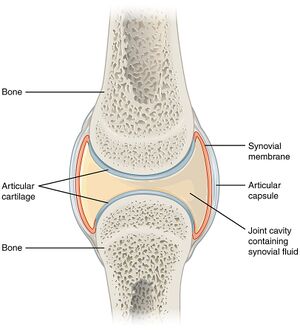
Synovial Joint
The cardinal feature of a synovial joint is that it is capable of substantial movement, such as with sliding in bending. This is in contrast to fibrocartilaginous and cartilaginous joints where the amplitude of movement is significantly lower.
Overview of Synovial Joint Structure
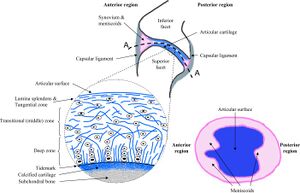
Joint Space: There must be some form of space between the two bones which allows the synovial joint to move. The space is quite narrow. The bones may be shaped in such a way to allow certain movements. For example flat surfaces allow sliding.
Cartilage: The most common effect that occurs at the joint is compression. When muscles act on the joint to move the joint they also exert a compression load across the joint space. The two bones are therefore subjected to phasic (intermittent) compression. Bones on their own are not well designed for phasic loads, but rather are better suited towards static loads. To protect against intermittent compression forces, the joint surfaces are lined with cartilage which provides a cushion or buffer. Cartilage is softer and somewhat more resilient than bone and can dissipate compression forces.
Synovial Fluid: A second hazard is friction. With movement in a gliding fashion, there is friction, which could result in stripping of the cartilage layers. To protect against friction the joint contains synovial fluid. This allows gliding movements between the joint surfaces. The synovial fluid layer is only one molecule thick, which is enough to provide the required anti-friction effects.
Synovial Membrane: The next design issue is that the synovial fluid has to be contained within the joint space and maintained at a suitable quality. Synovial membrane provides these functions. This structure is a sleeve of tissue that surrounds the joint space peripherally, and encloses the space in a thin membrane. The cells of the synovial membrane maintain the quality of the synovial fluid by removing debris and recycling used components back into the bloodstream.
Synovial Membrane Blood Vessels: The blood vessels located on the outer aspect of the synovial membrane have the role of synovial fluid production. Water and protein passes from the blood vessels, across the synovial membrane, and into the joint space. Various cells within the synovial membrane modify the synovial fluid to give the required structure.
Joint Capsule: The synovial membrane is delicate and is easily torn. It is supported on its outer surface by a joint capsule. This is relatively strong fibrous tissue that surrounds the joint space as another sleeve. The synovial membrane extends from the edge of the articular cartilage of one bone to the edge of the articular cartilage of the opposing bone. The capsule attaches further up along the neck of the two opposing bones. The main role of the capsule is protection of the synovial membrane, but also provides some mechanical stability.
Inclusions: Synovial joints can have intra-articular inclusions. A fibro-adipose meniscoid is a washer-like extension of the synovial membrane and capsule that extends into the joint cavity. The meniscoid has fatty tissue, with loose collagen and blood vessels at its core, coated by an extension of the synovial membrane. The function of the meniscoid is to subdivide the joint into two cavities. This results in lubricating fluid being present within each compartment.
Meniscoids are very common, and tend to be found in joints that have substantial sliding movements. During sliding the joint essentially subluxes, and there is unopposed cartilage. The meniscoid leaves the joint cavity and maintains the lubricating layer on the unopposed cartilage. When the joint returns to its neutral position, it does so with the joint surfaces having their lubricating layer being kept in place., and the meniscoid then re-enters the joint cavity.
Ligaments: The joint can be reinforced externally by ligaments. Ligaments may blend with the outer surface of the capsule, or stand alone leaving a space between the deep surface of the ligament and the capsule. Ligaments aren't an essential component of synovial joints, but are a common feature. The function of ligaments are to stabilise the joint against undesired movements.
Blood Vessels, Lymphatics, Nerves: The tissues of the joints have a blood supply with an arterial and venous supply. Lymphatic vessels drain excess fluid from the joint or synovial space. A nerve supply endows the joint and ligaments which monitor position and provide an alerting mechanism against threatened damage if there is excessive strain.
Articular Cartilage
- Main article: Articular Cartilage
Articular cartilage is a tissue that can resist, absorb, dissipate, and transmit intermittent compression. This is in contrast to bone which is better at resisting static compression. The cartilage retains its form and remains available for the next phase of compression. It also provides a smooth surface over which a joint can glide.
Articular cartilage is on average 2 to 4mm thick (retropatellar up to 7 to 8mm), and it doesn't have blood vessels, nerves, or lymphatics.
Synovial Membrane
Intima and Subintima
The term synovium refers to the soft tissue lining of diarthrodial joints, tendon sheaths, and bursae. It contains a surface layer called the intima, and underlying tissue called the subintima. Between the intimal surfaces is a small amount of fluid that is usually rich in hyaluronic acid. The synovium provides a non-adherent surface between tissue elements.[2]
The intima contains macrophages and fibroblasts and is two to three layers of cells thick. The cells aren't continuous like epithelium. Between them runs an amorphous matrix. The gaps between the cells allow easy communication through the intima.
The subintima consists of a loose network of collagen fibres; blood vessels; fat globules; and a variety of cells including mast cells, fibroblasts, and macrophages.
The blood vessels within the subintima produce most of the components by volume of synovial fluid. There is a transudate of fluid and proteins that passes into the joint space to start to produce synovial fluid..
Synovial macrophages
These are also known as macrophage-like synoviocytes (MLS), or type A synoviocytes. These are essentially macrophages. Previously they were thought to arise from bone marrow, but in reality they are derived from embryonic precursor cells and maintained by independent slow proliferation. [3]
They remove debris from the synovial fluid such as degraded aggrecans and other material that interfere with the lubricating property.
They also produce prostaglandins that can affect vasodilation or constriction of the subintimal blood vessels, thereby regulating the production of synovial fluid. For example in inflamed joints, prostaglandin production results in an effusion.
Synovial lining macrophages share certain features in common with epithelial cells. They express tight junction proteins, and provide an anti-inflammatory barrier around the joint that impairs immune cell traffic in a steady state. During arthritis this barrier "cracks" open.[4] Macrophages make up the minority of cells in normal intima, except in inflammatory arthritis where they make up 80% of the intima.[4]
These cells are also involved in the immune system as antigen presenting cells.
Synovial fibroblasts
These are also known as fibroblast-like synoviocytes (FLS), or type B synoviocytes. They are more abundant than synovial macrophages. They are thought to arise from mesenchymal stem cells. [3]
Fibroblasts produce inhibitors of phagocytic enzymes that are in turn produced by macrophages, and thereby prevent excessive activity.
Fibroblasts also secrete lubricin, the obsolete term for this was lubricating glycoprotein (LGP). It is also known as superficial zone protein. Lubricin is the cardinal component of synovial fluid and provides an anti-friction property. Hyaluronic acid and proteins on their own do not have an anti-friction property. Lubricin is also expressed by superficial zone chondrocytes and to a lesser extent intermediate zone chondrocytes.[5]
These cells also produce hyaluronan (note previously thought that this was produced by macrophages).[4]
FLS are involved in many pathological aspects of rheumatoid arthritis and promote synovitis, pannus growth, and cartilage/bone destruction.
Joint Lubrication
- See also: Cartilage Biomechanics
The ability of synovial fluid to lubricate the surface of cartilage depends on Lubricin (superficial zone protein), a glycoprotein located on the surface of the synovium and cartilage.
Hyaluronan is the main factor that is responsible for retaining a constant volume of fluid during exercise. The fluid cushions the synovial tissue and acts as a reservoir for lubricant for the cartilage. Mechanical stimulation of synovial fibroblasts is likely a key factor for stimulating the synthesis of hyaluronan. So when there is a large volume of synovial fluid, there is decreased mechanical stimulation and hence reduced synthesis, and vice versa.
Joint effusions can be created by two mechanisms, but they are not necessarily distinct. Osteoarthritis can display both mechanisms.
- Mechanical irritation: such as in osteoarthritis, there is excessive production of hyaluronan by synovial fibroblasts through frictional forces.
- Synovitis: this occurs through the accumulation of exudate, i.e. inflammatory oedema through increased vascular permeability.
List of Synovial Joints
| Acromioclavicular Joint | Joint type: Planar Joint | Bones: Clavicle, Scapula | Ligaments: Coracoclavicular, coracoacromial, superior acromioclavicular, and inferior acromioclavicular ligaments. | Muscles: No muscles directly act on this joint. | Innervation: Axillary, suprascapular, and lateral pectoral nerves | Vasculature: Suprascapular and thoracoacromial arteries | ROM: Upward rotation: 30 degrees, external rotation:8 degrees | Volume: 2mL |
| Atlanto-axial Joint | Joint type: Pivot Joint | Bones: C1 (Atlas), C2 (Axis) | Innervation: C2 | ROM: Rotation ~45° each way, flexion-extension ~10° each way, and lateral flexion ~5° each way | ||||
| Atlanto-occipital Joint | Joint type: Condyloid Joint | Bones: C1 (Atlas), Occiput | Ligaments: Two articular capsules, posterior atlanto-occipital membrane, anterior atlanto-occipital membrane | Muscles: Flexion by longi capitis and recti capitis anteriores; extension by recti capitis posteriores major and minor, the obliquus capitis superior, the semispinalis capitis, splenius capitis, sternocleidomastoid, and upper fibres of the trapezius. | Innervation: C1 | Vasculature: Anastomosis between the deep cervical, occipital and vertebral arteries. | ROM: 3.5 flexion, 21 extension, 10.9 lateral flexion each way, 6.7 rotation each way | |
| Cervical Zygapophyseal (Facet) Joint | Joint type: Planar Joint | |||||||
| Distal Radioulnar Joint | Joint type: Pivot Joint | Bones: Radius, Ulna | Ligaments: Triangular, anterior distal radioulnar, and posterior distal radioulnar ligaments | Muscles: Pronation: pronator quadratus, pronator teres; Supination: supinator, biceps brachii | Innervation: Anterior and posterior interosseous nerves | Vasculature: Anterior and posterior interosseous arteries | ||
| Elbow Joint | Joint type: Hinge Joint | Bones: Radius, Ulna, Humerus | Ligaments: Capsule, medial and lateral collateral ligaments, oblique cord, quadrate ligament | Innervation: Radial, ulnar, median, and musculocutaneous nerves | Vasculature: Anastomotic arcades formed by branches of radial, ulnar, and brachial arteries. | |||
| First Carpometacarpal Joint (Trapeziometacarpal Joint) | Joint type: Saddle Joint | Bones: Metacarpal, Trapezium | Ligaments: Capsule, anterior oblique, ulnar collateral, first intermetacarpal, posterior oblique, dorsoradial ligaments. | Innervation: Lateral antebrachial cutaneous nerve, palmar cutaneous branch of the median nerve, superficial radial nerve | Vasculature: First dorsal metacarpal branch of the radial artery | ROM: 53° of flexion/extension, 42° of abduction/adduction, and 17° of rotation | ||
| Glenohumeral Joint | Joint type: Ball and Socket Joint | Bones: Humerus, Scapula | Ligaments: Capsule, glenohumeral, coracohumeral and transverse humeral ligaments | Muscles: abduction: deltoid assisted by the supraspinatus; adduction: short scapular muscles (except supraspinatus) when the deltoid relaxes. Assisted by the pectoralis major and latissimus dorsi; flexion: clavicular head of the pectoralis major and the anterior fibres of the deltoid, assisted by the coracobrachialis and biceps; extension: latissimus dorsi, posterior fibres of the deltoid and the long head of the triceps; rotation: lateral rotation: infraspinatus and teres minor, medial rotation: subscapularis and teres major | Innervation: suprascapular, subscapular, axillary and lateral pectoral nerves | Vasculature: anterior and posterior humeral circumflex, and subscapular arteries | ROM: arm flexion, extension, adduction, abduction, and internal and external rotation | |
| Hip Joint | Joint type: Ball and Socket Joint | Bones: Ilium, Femur | Ligaments: Ischiofemoral, iliofemoral, pubofemoral, transverse acetabular, and ligamentum teres | Muscles: 27 musculotendinous units are involved in hip function | Innervation: Femoral, obturator and superior gluteal nerves, and nerve to quadratus femoris | Vasculature: Branches of the medial and lateral circumflex femoral, superior and inferior gluteal arteries and obturator arteries | ROM: Flexion 140°, extension 20°, Internal rotation 30°, external rotation 40°, abduction 50°, adduction 30° | Volume: 1-10mL |
| Interphalangeal Joints (Foot) | Joint type: Hinge Joint | Bones: Proximal Phalanx (Foot), Distal Phalanx (Foot) | ||||||
| Knee Joint | Joint type: Saddle Joint, Hinge Joint | Bones: Tibia, Femur, Patella | Innervation: Popliteal nerve, tibial nerve | Vasculature: Genicular branches of the popliteal artery | ROM: Mainly sagittal plane: 3° of hyperextension to 155° of flexion | |||
| Lumbar Zygapophyseal (Facet) Joint | Joint type: Planar Joint | Bones: Vertebra | Ligaments: Capsular Ligament | Innervation: Medial Branches of the Dorsal Rami | Vasculature: Branches of Lumbar Arteries | ROM: Limited Flexion, Extension, Lateral Flexion, and Rotation | ||
| Metacarpophalangeal Joint | Joint type: Condyloid Joint | Bones: Metacarpal, Proximal Phalanx (Hand) | Ligaments: Capsule, two collateral ligaments, palmar (volar) ligament | Innervation: Digital nerves from the ulnar and median nerves | Vasculature: Deep digital arteries from the superficial palmar arch | |||
| Metatarsophalangeal Joints | Joint type: Condyloid Joint | Bones: Metacarpal, Proximal Phalanx (Foot) | Ligaments: Capsule, collateral ligamentous complexes, plantar plate. For great toe also sesamoid-phalangeal ligaments. | Muscles: flexor digitorum longus, flexor digitorum brevis, extensor digitorum longus, extensor digitorum brevis, flexor digiti minimi brevis, abductor digiti minimi, dorsal and plantar Interossei, lumbricals | Innervation: Digital nerves from the ulnar and median nerves | Vasculature: Deep digital arteries from the superficial palmar arch | ||
| Proximal Radioulnar Joint | Joint type: Pivot Joint | Bones: Radius, Ulna | Ligaments: Annular ligament | Innervation: Articular branches of the musculocutaneous, median, and radial nerve | Vasculature: Radial portion of the peri-articular arterial anastomosis of the elbow joint | |||
| Radiocarpal Joint | Joint type: Condyloid Joint | Bones: Radius, Ulna, Scaphoid, Lunate, Triquetrum | Ligaments: Volar: radial collateral ligament to styloid process, radioscaphocapitate, ligament radiolunate ligament, radioscapholunate ligament; Dorsal: radioscaphoid ligament, radiolunate ligament, radiotriquetral ligament | Muscles: flexor digitorum superficialis, flexor digitorum profundus, palmaris longus, flexor carpi radialis and ulnaris, extensor carpi radialis longus and brevis, extensor carpi ulnaris, extensor digitorum, flexor carpi ulnaris, extensor carpi ulnaris, extensor carpi radialis longus and brevis, flexor carpi radialis | Innervation: anterior interosseous nerve arising from median nerve (C5-T1), posterior interosseous nerve arising from radial nerve (C7-C8) | Vasculature: Palmar carpal arch (from palmar carpal branches of radial and ulnar arteries, reinforced by anterior interosseous artery and penetrating deep branches of deep palmar arch), dorsal carpal arch (formed by dorsal carpal branches of radial and ulnar arteries, reinforced by anterior and posterior interosseous arteries) | ||
| Sacroiliac Joint | Bones: Ilium, Sacrum | Ligaments: Anterior sacroiliac, interosseous sacroiliac, posterior sacroiliac, long posterior sacroiliac, sacrotuberous, sacrospinous, and iliolumbar ligaments. | Innervation: Posterior joint lateral branches of the posterior rami of L5-S4. Anterior joint L4-S3 (+/- L3, sacral plexus, superior gluteal nerve) | Vasculature: Median sacral artery and the lateral sacral branches of the internal iliac artery | ROM: 0-2° | Volume: 1 - 1.5 mLs | ||
| Sternoclavicular Joint | Joint type: Saddle Joint | Bones: Clavicle, Rib 1, Manubrium | Ligaments: Sternoclavicular, costoclavicular, interclavicular ligs. | Innervation: Medial supraclavicular (C3-4) and subclavian (C5-6) nn. | Vasculature: Internal thoracic and suprascapular aa. (branches of the subclavian a.) | ROM: 35° in the horizontal and coronal planes, 70° range of motion anteroposteriorly, 50° of rotation along its long axis. | ||
| Talocalcaneal Joint (Subtalar Joint) | Joint type: Planar Joint | Bones: Talus, Calcaneus | Ligaments: Multiple, interosseous talocalcaneal ligament is most important | Innervation: Medial plantar, lateral plantar, and deep fibular nerves | Vasculature: Posterior tibial and fibular arteries | ROM: Equal components of inversion/eversion and abduction/adduction. | ||
| Tibiotalar Joint (Talocrural Joint) | Joint type: Hinge Joint | Bones: Tibia, Fibula, Talus | Ligaments: Syndesmosis, medial collateral ligaments, lateral collateral ligaments | Innervation: tibial nerve, deep peroneal nerve | Vasculature: anterior and posterior tibial arteries, peroneal artery | ROM: 10° to 20° of dorsiflexion, 40° to 55° of plantarflexion | Volume: 16-30 mL |
Resources
See Also
References
- ↑ Jaumard, Nicolas V et al. “Spinal facet joint biomechanics and mechanotransduction in normal, injury and degenerative conditions.” Journal of biomechanical engineering vol. 133,7 (2011): 071010. doi:10.1115/1.4004493
- ↑ Smith, Malcolm D. “The normal synovium.” The open rheumatology journal vol. 5 (2011): 100-6. doi:10.2174/1874312901105010100
- ↑ 3.0 3.1 Tu J, Hong W, Zhang P, Wang X, Körner H, Wei W. Ontology and Function of Fibroblast-Like and Macrophage-Like Synoviocytes: How Do They Talk to Each Other and Can They Be Targeted for Rheumatoid Arthritis Therapy? Front Immunol. 2018 Jun 26;9:1467. doi: 10.3389/fimmu.2018.01467. PMID: 29997624; PMCID: PMC6028561.
- ↑ 4.0 4.1 4.2 Collison, J. Synovial macrophages shield the joints. Nat Rev Rheumatol 15, 573 (2019). https://doi.org/10.1038/s41584-019-0295-6
- ↑ Jay GD, Waller KA. The biology of lubricin: near frictionless joint motion. Matrix Biol. 2014 Oct;39:17-24. doi: 10.1016/j.matbio.2014.08.008. Epub 2014 Aug 27. PMID: 25172828.
Literature Review
- Reviews from the last 7 years: review articles, free review articles, systematic reviews, meta-analyses, NCBI Bookshelf
- Articles from all years: PubMed search, Google Scholar search.
- TRIP Database: clinical publications about evidence-based medicine.
- Other Wikis: Radiopaedia, Wikipedia Search, Wikipedia I Feel Lucky, Orthobullets,